Curcumin 图表
13 来自同行评审研究的图表
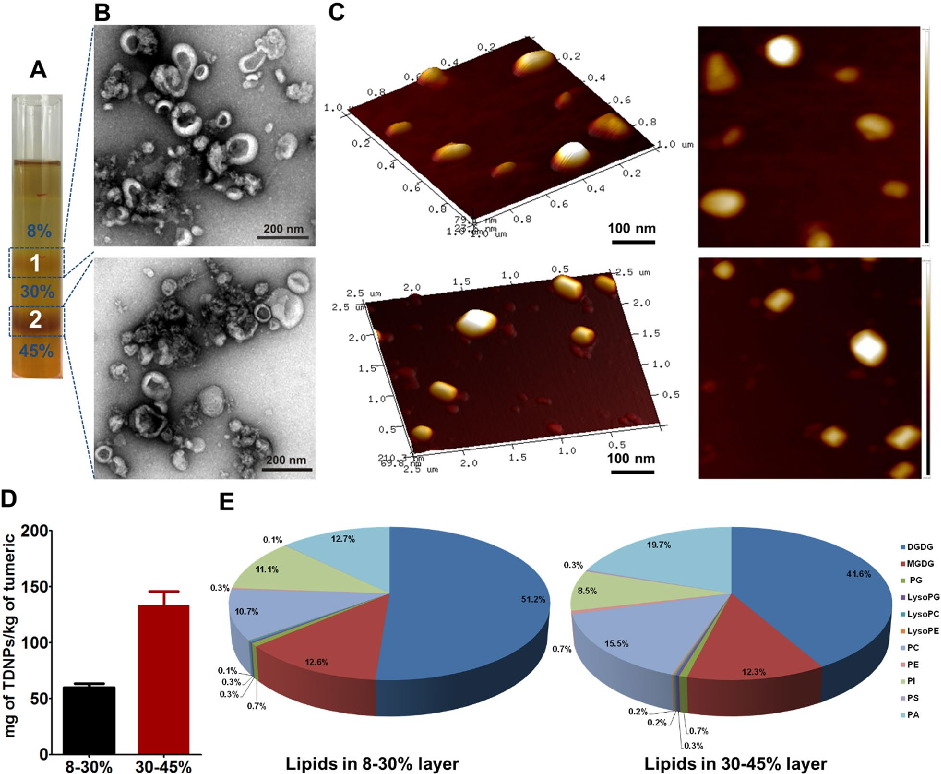
Characterization of turmeric-derived nanoparticles reveals two distinct bands (TDNPs 1 and TDNPs 2) at the 8%/30% and 30%/45% sucrose gradient interfaces, respectively. TDNPs 2 demonstrate appropriate size distribution and surface charge for oral drug delivery applications.
Oral administration of turmeric-derived exosome-like nanovesicles with anti-inflammatory and pro-resolving bioactions for …
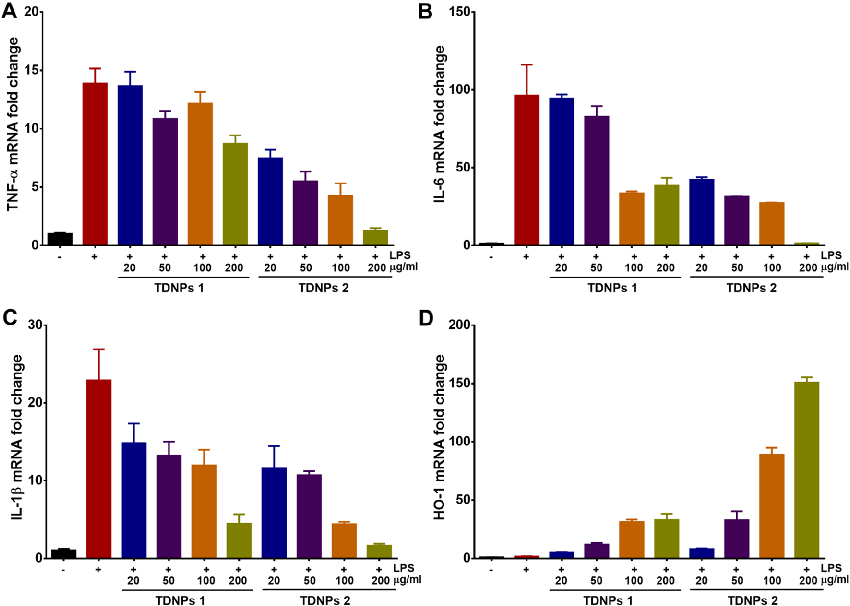
In vitro assessment of turmeric-derived nanovesicles demonstrates anti-inflammatory activity, including suppression of pro-inflammatory cytokine production in activated macrophages. Dose-dependent reductions in TNF-alpha and IL-6 secretion are observed.
Oral administration of turmeric-derived exosome-like nanovesicles with anti-inflammatory and pro-resolving bioactions for …
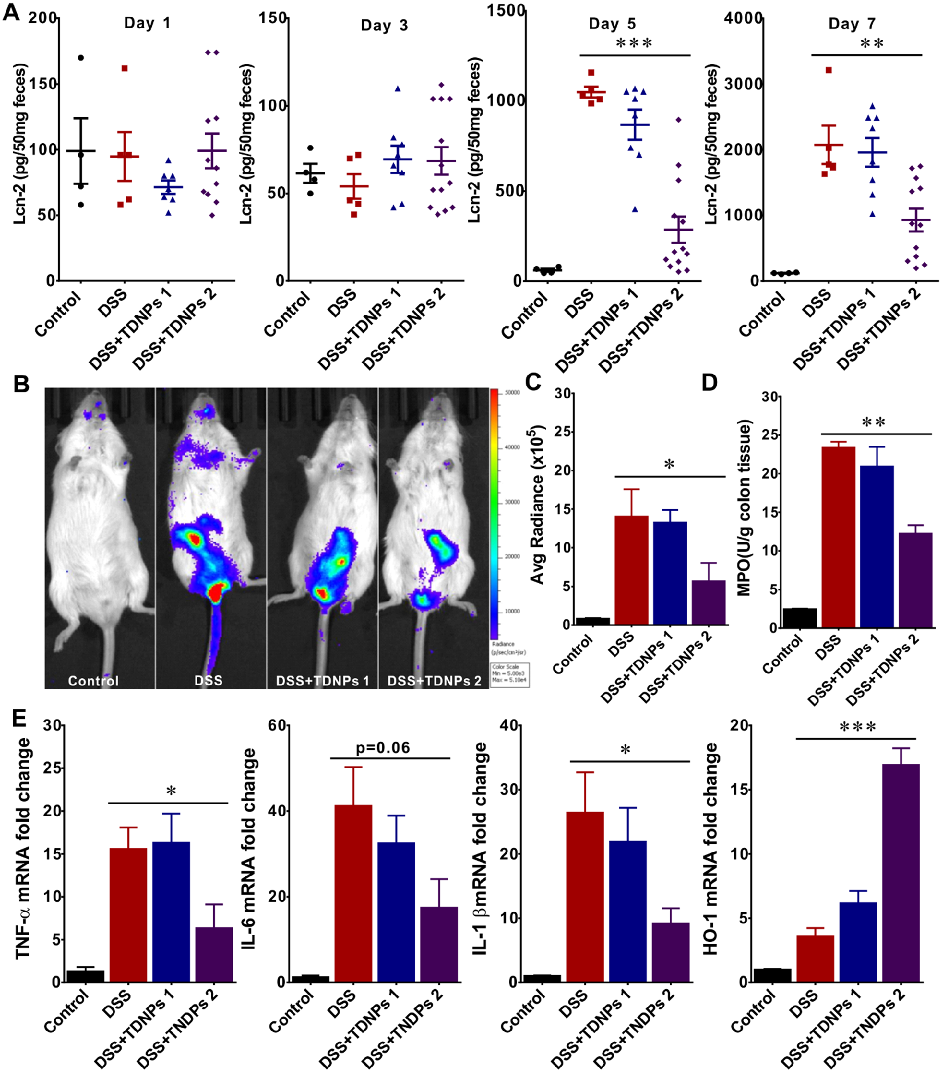
Oral TDNPs 2 administration significantly attenuates disease activity index scores and colon shortening in DSS-induced colitis mice. Body weight recovery is also improved compared to untreated colitis controls.
Oral administration of turmeric-derived exosome-like nanovesicles with anti-inflammatory and pro-resolving bioactions for …
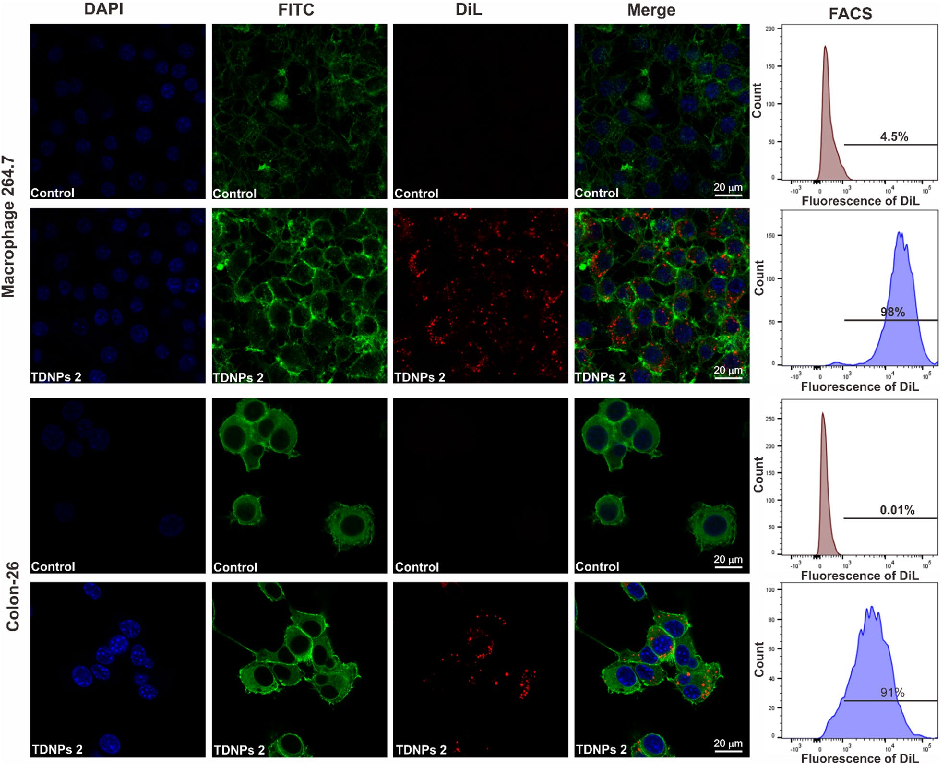
Intestinal permeability assessment indicates that TDNPs 2 treatment preserves gut barrier integrity in colitis mice. Tight junction protein expression, including ZO-1 and occludin, is maintained at near-normal levels.
Oral administration of turmeric-derived exosome-like nanovesicles with anti-inflammatory and pro-resolving bioactions for …
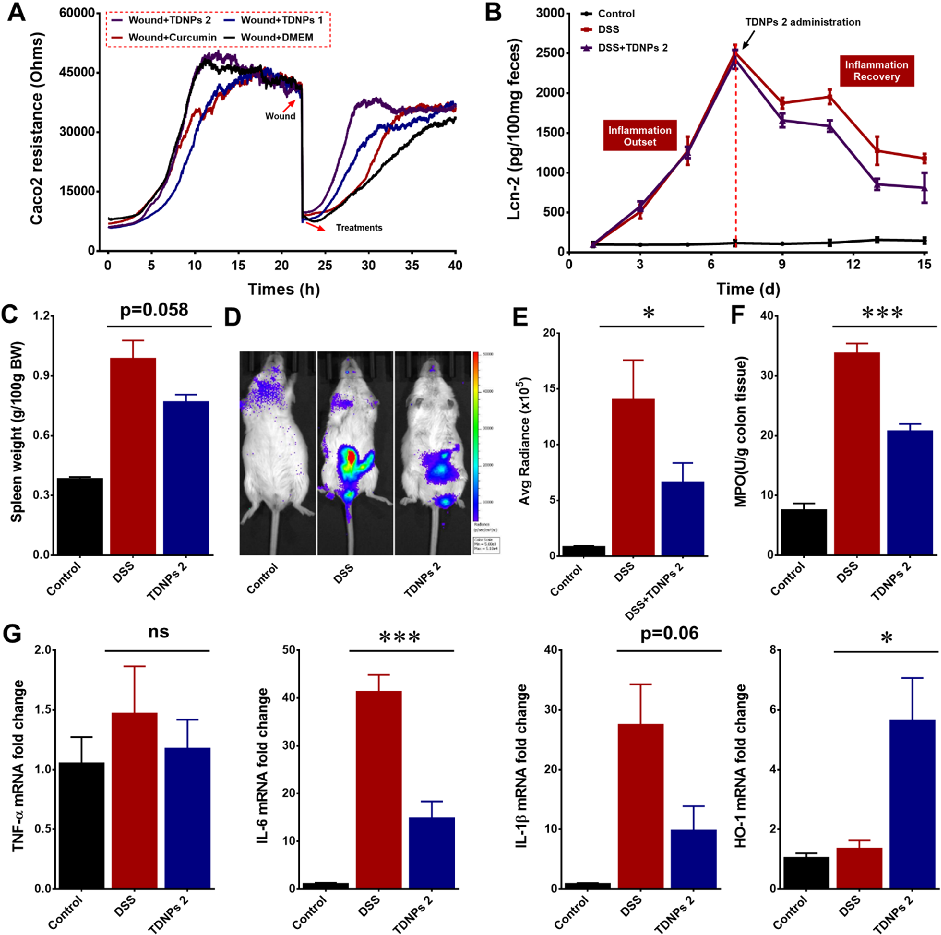
Wound healing assays and fecal lipocalin-2 quantification demonstrate that TDNPs 2 accelerate resolution of intestinal inflammation. Lcn-2 levels, a sensitive marker of intestinal inflammation, decrease significantly with treatment.
Oral administration of turmeric-derived exosome-like nanovesicles with anti-inflammatory and pro-resolving bioactions for …
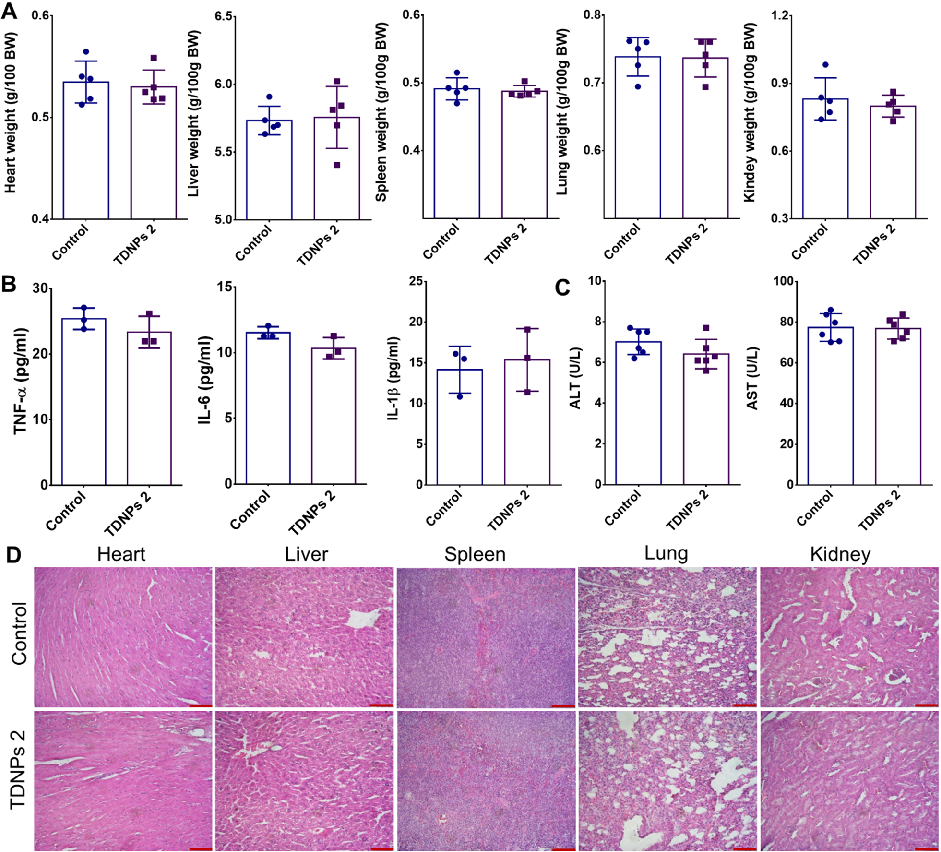
Biocompatibility evaluation shows no significant changes in vital organ weights, pro-inflammatory cytokines, or liver function indicators in TDNPs 2-treated mice. H&E staining of major organs confirms absence of toxicity.
Oral administration of turmeric-derived exosome-like nanovesicles with anti-inflammatory and pro-resolving bioactions for …
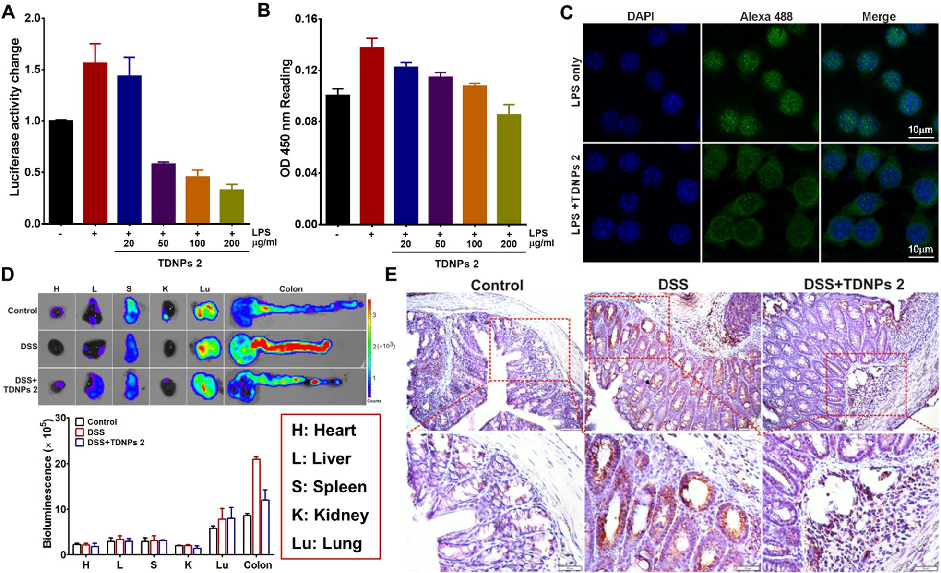
TDNPs 2 exert their protective effect at least partly through inactivation of the NF-kB signaling pathway. Reduced phospho-NF-kB p65 expression and decreased nuclear translocation indicate suppression of this key inflammatory cascade.
Oral administration of turmeric-derived exosome-like nanovesicles with anti-inflammatory and pro-resolving bioactions for …
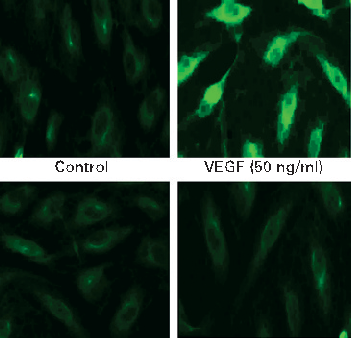
COX-2 protein expression is upregulated by VEGF stimulation in intestinal endothelial cells, and curcumin effectively blocks this induction. Prostaglandin E2 production follows a similar pattern of inhibition.
Curcumin inhibits VEGF-mediated angiogenesis in human intestinal microvascular endothelial cells through COX-2 …

MAPK signaling pathway activation by VEGF is attenuated by curcumin in a time- and dose-dependent manner. Phosphorylation of ERK, p38, and JNK is markedly reduced in curcumin-treated endothelial cells.
Curcumin inhibits VEGF-mediated angiogenesis in human intestinal microvascular endothelial cells through COX-2 …
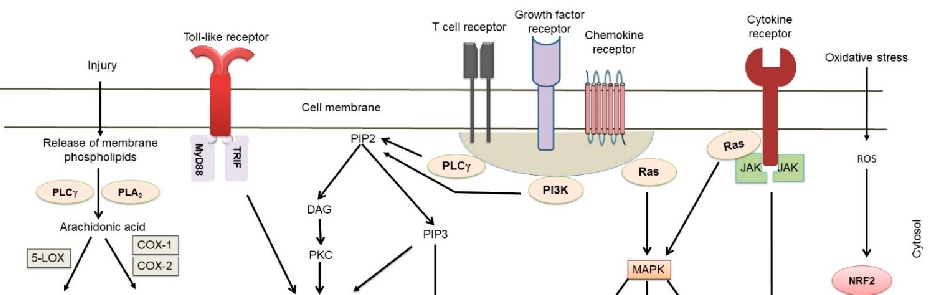
In vivo models of autoimmune diseases have demonstrated therapeutic efficacy of various natural compounds. This figure presents preclinical evidence from animal models of rheumatoid arthritis, multiple sclerosis, or inflammatory bowel disease treated with natural products.
The Anti-Inflammatory and Immunomodulatory Activities of Natural Products to Control Autoimmune Inflammation.
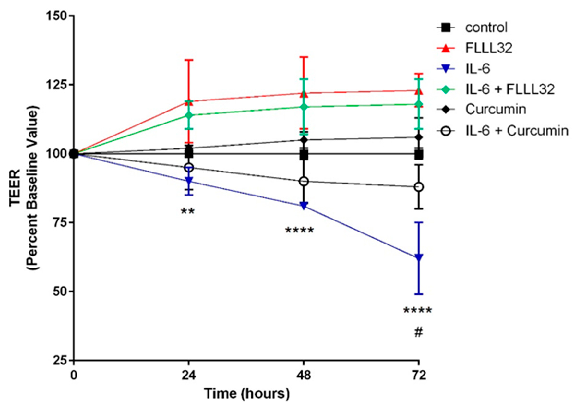
FLLL32 (a curcumin analogue) and curcumin both protect against IL-6-induced reduction of transepithelial electrical resistance (TEER) in T84 cell monolayers. This graph shows that curcumin preserves intestinal barrier integrity by counteracting cytokine-mediated tight junction disruption over 72 hours.
Curcumin and Intestinal Inflammatory Diseases: Molecular Mechanisms of Protection.
Curcumin's effects on intestinal tight junction proteins have been demonstrated in multiple experimental models. This figure presents protein expression or immunofluorescence data showing curcumin-mediated preservation of barrier function.
Curcumin and Intestinal Inflammatory Diseases: Molecular Mechanisms of Protection.
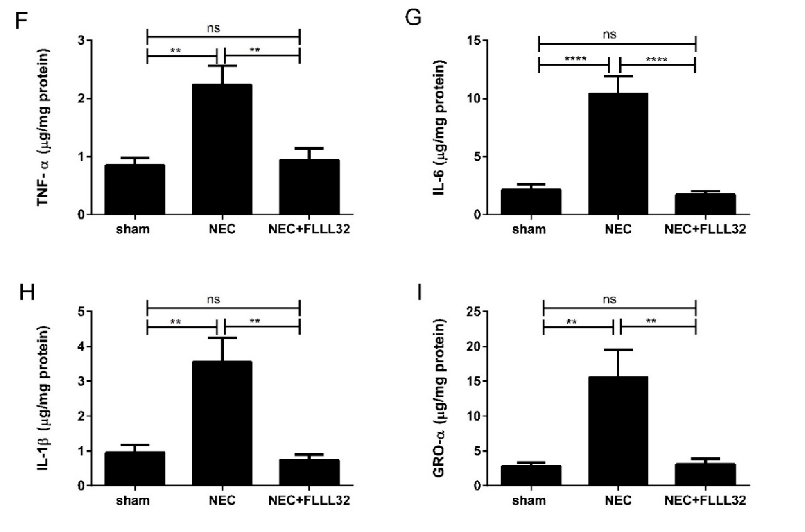
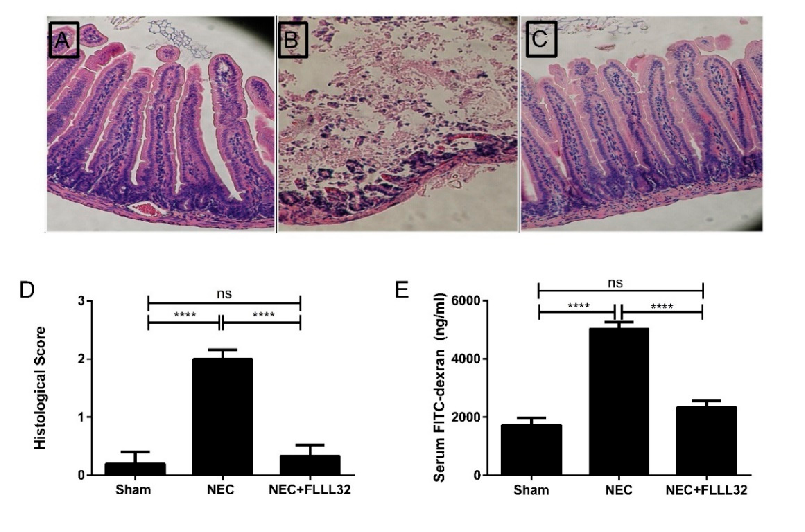
Animal models of necrotizing enterocolitis and colitis respond favorably to curcumin treatment. This figure presents in vivo data on curcumin's protective effects in experimental intestinal inflammation.
Curcumin and Intestinal Inflammatory Diseases: Molecular Mechanisms of Protection.