Evaluation of the Efficacy of Kombucha-Based Drink Enriched with Inulin and Vitamins for the Management of Constipation-Predominant Irritable Bowel Syndrome in Females: A Randomized Pilot Study.
Study Design
- 연구 유형
- Randomized Controlled Trial
- 대상 집단
- Patients with constipation-predominant IBS
- 중재
- Evaluation of the Efficacy of Kombucha-Based Drink Enriched with Inulin and Vitamins for the Management of Constipation-Predominant Irritable Bowel Syndrome in Females: A Randomized Pilot Study. 220 mL
- 대조군
- control
- 일차 결과
- IBS-C symptom improvement
- 효과 방향
- Positive
- 비뚤림 위험
- Moderate
Abstract
BACKGROUND: Constipation-predominant irritable bowel syndrome (IBS-C) mainly affects females, and dietary interventions for symptom relief often yield poor results because of low patient adherence. The development of functional food products enriched with dietary fibers may increase patients' adherence to a healthy diet and relieve IBS-С symptoms. OBJECTIVE: This proof-of-concept, open-label, randomized controlled pilot study is aimed to evaluate the efficacy of kombucha enriched with inulin and vitamins in females with IBS-C. METHODS: Forty females with IBS-C were randomly assigned to receive either 220 mL of kombucha enriched with inulin (2.53 g/220 mL) and vitamins (B1 - 0.59 mg, B2 - 0.55 mg, B3 - 5.9 mg, B6 - 0.7 mg, and folic acid - 81.4 μg/220 mL) or water for 10 d. Stool frequency, Bristol stool scale score (BSSS), and abdominal symptoms were evaluated using a 5-point Likert scale on days 5, 9 and 14 of the study. The palatability of the drink was assessed using a visual analog scale. RESULTS: After 10 d, the kombucha group showed a significant increase in stool frequency (0.60 ± 0.31-0.85 ± 0.19 times/d; P = 0.004) compared with the control (0.63 ± 0.33 compared with 0.72 ± 0.28; P = 0.6). The mean values of the BSSS increased in the kombucha group (3.0 ± 1.2-4.4 ± 1.0; P = 0.001), whereas they remained unchanged in the control (2.9 ± 1.2 compared with 3.4 ± 1.2; P = 0.6). The kombucha group also experienced a significant decrease in the feeling of incomplete bowel emptying (1.88 ± 0.78 compared with 1.41 ± 0.56 points; P = 0.015), which was not observed in the control group. CONCLUSIONS: Short-term consumption of kombucha enriched with inulin and vitamins was associated with an increase in stool frequency, an improvement in the BSSS, and a reduction in the feeling of incomplete bowel emptying in females with IBS-C. Further large-scale clinical trials investigating the efficacy of kombucha enriched with inulin and vitamins in patients with IBS-C are warranted to prove the observed effects. TRIAL REGISTRATION NUMBER: This trial was registered at clinicaltrials.gov as NCT05164861 (==https://clinicaltrials.gov/study/NCT05164861?term=NCT05164861&rank=1; registered on 18 December, 2021).
요약
Short-term consumption of kombucha enriched with inulin and vitamins was associated with an increase in stool frequency, an improvement in the BSSS, and a reduction in the feeling of incomplete bowel emptying in females with IBS-C.
Full Text
Current Developments in Nutrition 7 (2023) 102037
journal homepage: https://cdn.nutrition.org/
Original Research
Evaluation of the Efficacy of Kombucha-Based Drink Enriched with Inulin and Vitamins for the Management of Constipation-Predominant Irritable Bowel Syndrome in Females: A Randomized Pilot Study
Vasily A Isakov 1,*, Vladimir I Pilipenko1, Alina V Vlasova 1, Alla A Kochetkova 2
- 1 Department of Gastroenterology & Hepatology, Federal Research Centre of Nutrition, Biotechnology and Food Safety, Moscow, Russia;
- 2 Laboratory of Food Biotechnology and Foods for Special Dietary Uses, Federal Research Centre of Nutrition, Biotechnology and Food Safety, Moscow, Russia
A B S T R A C T
Background: Constipation-predominant irritable bowel syndrome (IBS-C) mainly affects females, and dietary interventions for symptom relief often yield poor results because of low patient adherence. The development of functional food products enriched with dietary fibers may increase patients’ adherence to a healthy diet and relieve IBS-С symptoms.
Objective: This proof-of-concept, open-label, randomized controlled pilot study is aimed to evaluate the efficacy of kombucha enriched with inulin and vitamins in females with IBS-C.
Methods: Forty females with IBS-C were randomly assigned to receive either 220 mL of kombucha enriched with inulin (2.53 g/220 mL) and vitamins (B1 0.59 mg, B2 0.55 mg, B3 5.9 mg, B6 0.7 mg, and folic acid 81.4 μg/220 mL) or water for 10 d. Stool frequency, Bristol stool scale score (BSSS), and abdominal symptoms were evaluated using a 5-point Likert scale on days 5, 9 and 14 of the study. The palatability of the drink was assessed using a visual analog scale.
Results: After 10 d, the kombucha group showed a significant increase in stool frequency (0.60 0.31–0.85 0.19 times/d; P ¼ 0.004) compared with the control (0.63 0.33 compared with 0.72 0.28; P ¼ 0.6). The mean values of the BSSS increased in the kombucha group (3.0 1.2 4.4 1.0; P ¼ 0.001), whereas they remained unchanged in the control (2.9 1.2 compared with 3.4 1.2; P ¼ 0.6). The kombucha group also experienced a significant decrease in the feeling of incomplete bowel emptying (1.88 0.78 compared with 1.41 0.56 points; P ¼ 0.015), which was not observed in the control group.
Conclusions: Short-term consumption of kombucha enriched with inulin and vitamins was associated with an increase in stool frequency, an improvement in the BSSS, and a reduction in the feeling of incomplete bowel emptying in females with IBS-C. Further large-scale clinical trials investigating the efficacy of kombucha enriched with inulin and vitamins in patients with IBS-C are warranted to prove the observed effects.
Trial registration number: This trial was registered at clinicaltrials.gov as NCT05164861 ( https://clinicaltrials.gov/study/ NCT05164861?term¼NCT05164861&rank¼1; registered on 18 December, 2021).
Keywords: females’s health, fermented beverages, dietary fibers, irritable bowel syndrome, constipation, kombucha, inulin, Bristol stool scale score, stool frequency
Introduction
Irritable bowel syndrome (IBS) is a common functional gastrointestinal disorder that affects ~10%–20% of the population in economically developed countries. Among IBS cases,
approximately one-third are associated with constipation and classified as constipation-predominant irritable bowel syndrome (IBS-C) according to the ROME IV criteria [1]. IBS is more prevalent in females, with a female-to-male ratio of 2–2.5:1 among those seeking medical care [2]. Furthermore, a large
Abbreviations: BSSS, Bristol stool scale score; IBS, irritable bowel syndrome; IBS-C, constipation-predominant irritable bowel syndrome; VAS, visual analog scale.
* Corresponding author. E-mail address: [email protected] (V.A. Isakov).
https://doi.org/10.1016/j.cdnut.2023.102037 Received 24 July 2023; Received in revised form 5 November 2023; Accepted 9 November 2023; Available online 24 November 2023 2475-2991/© 2023 The Author(s). Published by Elsevier Inc. on behalf of American Society for Nutrition. This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/4.0/).
meta-analysis reported a pooled prevalence of IBS-C in females with IBS of 40%, compared with 21% in males with IBS [3], highlighting its significance in females's health. Although the exact cause of IBS is unknown, diet is considered one of the factors that can trigger or exacerbate symptoms [4,5]. Low intake of water and dietary fibers is associated with an increased risk of IBS-C, as dietary fibers increase fecal mass and colonic transit while retaining water in the colon and providing a stool-softening effect. Moreover, soluble dietary fibers, acting as prebiotics, have the potential to normalize the intestinal microbiota in patients with IBS when consumed in higher quantities [6,7].
Inulin, a fructan with prebiotic properties, can be extracted from various vegetables and fruits such as artichokes, chicory, dandelion leaves, and asparagus. Inulin's prebiotic activity has been extensively demonstrated in numerous studies, showing selective fermentation by bifidogenic bacteria [8,9]. Several meta-analyses have confirmed the positive effects of inulin on the colonic microbiome and stool frequency in patients with functional constipation and IBS-C [10–13]. The prescription of a diet rich in dietary fibers is a typical treatment approach for patients with IBS-C and has been proven to be effective [14]. However, follow-up studies have shown that only 30%–40% of patients adhere to dietary interventions [15,16]. To improve adherence, it is important to develop a diet that includes tasty foods with acceptable sensory qualities, allowing patients to maintain their nutritional habits while receiving the necessary amount of dietary fibers to alleviate IBS-C symptoms.
Functional drinks have gained popularity worldwide because of their appealing taste, and their consumption is not associated with health risks as has been demonstrated for regular intake of sugar-sweetened or artificially sweetened carbonated drinks [17]. Among functional drinks (sports drinks, fortified juices, diary-alternative drinks, etc.), kombucha has become the most popular in the last 10 y with a rapidly growing and expanding market [18]. It can easily be flavored with natural fruits and berries as well as enriched with different biologically active substances for health benefits. In line with this approach, we developed a kombucha-based drink enriched with inulin and vitamins [19]. The objective of this study was to clinically evaluate the efficacy of a nonalcoholic fermented pasteurized kombucha drink enriched with inulin and vitamins in females with IBS-C.
Materials
Participants
IBS-C females were recruited from the Gastroenterology andHepatologyDepartment,FederalResearchCentreofNutrition, Biotechnology, and Food Safety in Moscow, Russian Federation in 2021 to participate in a clinical study involving the kombucha drink.Thepilotstudyfollowedasingle-center,open-label,parallelgroup, randomized controlled trial design (NCT 05164861; registered on 18 December, 2021; https://clinicaltrials.gov/study/ NCT05164861?term¼NCT05164861&rank¼1). Patients with IBS-C were selected based on the following inclusion criteria (Figure 1):
Willingness to participate in the study, as indicated by a signed patient information sheet. Age ranging from 18 to 80 y old. Diagnosis of IBS with constipation based on ROME IV criteria. Agreement to refrain from taking laxatives during the study.
The criteria for excluding patients in the study were: Lack of desire to participate in the study. Unwillingness to comply with the necessary requirements to obtain accurate examination results. General conditions and the presence of severe concurrent conditions that could significantly impact the study results and data interpretation. Any food allergies or intolerances.
Participants were randomly assigned to a treatment sequence order using a computer-generated list provided by staff members who were not involved in the clinical assessment or data analyses.
Test product
The test product was a nonalcoholic pasteurized kombucha drink enriched with inulin and vitamins. The initial ingredients of the drink included drinking water, black tea, a freshly grown kombucha starter culture, black currant berries/juniper berries or strawberries/lime leaves or mango/passion fruit puree, inulin, and vitamins (B1, B2, B3, B6, and folic acid). To prepare the fermented drink, we used black Indian big leaf tea (Camellia Sinensis), sucrose, a symbiotic culture of bacteria, and yeast—SCOBY (Acetobacter spp., Gluconacetobacter spp., Komagataeibacter spp., Brettanomyces bruxellensis, Saccharomyces spp., Starmerella spp., Zygosaccharomyces spp.) (LiveBrew), frozen strawberry fruit and Kaffir lime leaves (provided by a local supermarket), and inulin. The vitamin premix RUS 28,174 (DSM Nutritional Products Europe Ltd.) containing 48,750 mg/kg of thiamine (Vitamin B1), 44,000 mg/kg of riboflavin (Vitamin B2), 479,998 mg/kg of niacin (Vitamin B3), 57,000 mg/kg of pyridoxine (Vitamin B6), and 7500 mg/kg of folic acid was used to fortify the drink. Flavoring agents were added to 1038 g of Kombucha base in the following ratio: Strawberry – 173.0 g and Kaffir lime leaf – 3.7 g. The ingredients were added in such a way that after filtration, the yield of the product was 1000 g [19].
During the production of the drink, 2 rounds of fermentation and pasteurization of the final product were performed. The effectiveness of the pasteurization process was confirmed through routine laboratory microbiological tests, including counts of mesophilic aerobic bacteria, yeasts and molds, total coliforms, and Escherichia coli. The full technology and production process of the kombucha drink enriched with inulin and vitamins was developed by us, and throughout the study period, the quality control of the drink was performed as we previously described [19].
One hundred milliliters of the drink after fermentation contained: carbohydrates – 2.57 g (including sucrose – 0.22 g, glucose 1.32 g, and fructose 1.03 g), inulin 1.15 g, vitamin B1 – 0.4 mg, B2 – 0.21 mg, B3 – 2.74 mg, B6 – 0.48 mg, and folic acid – 24.0 μg. Energy value/caloric content – 54 kJ/13 kcal [19].
Diet
Throughout the study period, all patients received the standard version of the diet, which was prepared in the hospital kitchen. The diet consisted of a normal amount of protein (85–90 g/d), fat (70–80 g/d), and carbohydrates (300–330 g/d). The caloric content of the diet ranged from 2170 to 2400 kcal. The fiber intake was set at 25 g/d (including the inulin from the tested drink), table salt at 6 g/d, and free liquid intake at 1.5–2.0 L. Boiled, stewed, and baked dishes were provided. The addition of the tested kombucha drink to the diet increased its caloric content by 28.6 kcal and carbohydrate content by 5.6 g. An example of a daily menu is presented in Supplemental Table 1.
Study design
This study was designed as a single-center, prospective, openlabel, randomized controlled trial to evaluate the effects of a nonalcoholic pasteurized fermented kombucha drink enriched with inulin and vitamins in 20 patients with constipation (defined as <1 spontaneous bowel movement in 3 d). The patients in the study group consumed a modified diet in which a 220 mL portion of the studied kombucha drink replaced their breakfast drink daily for a period of 10 d. After randomization, patients in the kombucha group may choose 1 of 3 flavors of the drink they will consume during the intervention phase of the study. The control group received a standard diet with a 220 mL portion of water replacing their breakfast drink during the same period. No one from the enrolled females used any kombucha drink before this study.
During the study, the sensory properties and tolerability of the product were assessed, along with any concomitant
complaints (dryness, bitterness in the mouth, belching with food/air, heartburn, heaviness in the stomach, abdominal pain, nausea, and flatulence). Stool frequency (number of bowel movements/d) and stool form (assessed using the Bristol stool scale) were evaluated on days 5, 9, and 14 (Figure 2). The sensory properties of the product were assessed using a 100 mm visual analog scale (VAS) ranging from “very tasty” to “absolutely tasteless” on days 5 and 14. Clinical safety parameters, including blood count, urine tests, and biochemical blood analysis (bilirubin, creatinine, blood urea nitrogen, alanine aminotransferase activity, aspartate aminotransferase activity, gammaglutamyltransferase activity, glucose, total protein, potassium, sodium, and iron) were assessed at the beginning and at the end of the study.
Ethics
All patients provided written informed consent before participating in the study. The study protocol and informed consent form were approved by the local ethics committee on 15 October, 2021. The amendment to the protocol of the clinical trial, which added the third flavor (mango/passion fruit) of the tested product, was approved by the local ethics committee on 29 November, 2021. The study was conducted in accordance with the latest Declaration of Helsinki. All authors had access to the study data, reviewed the manuscript, and approved the final version.
Statistics
Data analysis was performed using "SPSS Statistics for Windows, Version 23.0" software (IBM Corp.,). Descriptive statistics
Overall, by the end of the study, all patients in the kombucha group showed an improvement in general well-being, a decrease in the severity of clinical manifestations of the underlying disease, and an increase in stool frequency. There were no statistically significant differences between the 2 groups in terms of bitterness and dry mouth, heartburn, nausea, abdominal pain, and postprandial stomach heaviness. While there was no overall increase in the intensity of heartburn in the kombucha group (from 1.28 0.62 to 1.25 0.52 points on the Likert scale at the end of the study), 2 patients reported experiencing prolonged heartburn after consuming the mango–passion fruit-flavored kombucha drink, and 3 patients noted an exacerbation of preexisting heartburn.
- TABLE 1 Comparison of groups by age and BMI (M m)
- TABLE 2 Comparison of patient groups by severity of complaints according to Likert scale scores
methods were used to evaluate the sample indicators, and the data are presented as means and standard deviations. Participant characteristics were compared using the Wilcoxon rank sum test, Mann–Whitney U test, and χ2 test for categorical variables. Statistical significance was set at P < 0.05.
Results
Between the 5th and 9th days of consuming the kombucha drink, 7 of 20 patients (35%) in the kombucha group reported an increase in complaints of moderate abdominal distension, which may be indicative of the utilization of inulin, an added component in the drink, by the intestinal microflora. Although there were no significant changes in the severity of bloating (P ¼ 0.08), it was nearly completely resolved by the end of the study period in 5 of 7 patients (Figure 3).
A total of 52 participants were screened, and after excluding 12 individuals, 40 were enrolled in the study and randomly allocated to the kombucha and control groups. The groups were comparable in terms of age, gender, and BMI (Table 1). The main clinical manifestations of IBS-C in the patients included a feeling of incomplete emptying after defecation, bloating, abdominal pain, and postprandial stomach heaviness (Table 2).
From the 5th day of observation, the kombucha group showed a statistically significant decrease in the severity of
Complaints of patients Kombucha group (n ¼ 20) Control group (n ¼ 20)
Dry mouth 1.28 0.56 1.45 0.68 Heartburn 1.28 0.62 1.40 0.68 Mouth bitterness 1.40 0.59 1.35 0.58 Heaviness in the stomach after eating 1.53 0.69 1.80 0.89 Abdominal pain 1.28 0.56 1.65 0.58 Nausea 1.15 0.45 1.0 0 Bloating 1.6 0.64 1.75 0.9 Feeling of incomplete emptying 1.88 0.78 1.85 0.74 Stool frequency (times/d) 0.60 0.31 0.62 0.33 Bristol stool scale score 2.95 1.52 2.90 1.29
Data are presented as mean SD for normally distributed data.
incomplete bowel emptying (from 1.88 0.78 to 1.41 0.78 points on the Likert scale, P ¼ 0.015). In contrast, there were no significant differences in the intensity of the feeling of incomplete emptying in the control group (Figure 4).
Figure 5 illustrates the changes in stool frequency. In the kombucha group, there was a significant increase in stool frequency, from 0.60 0.31 to 0.85 0.19 times/d (P ¼ 0.004). To the contrary, in the control group, there was only a minimal increase of 0.3 times/d, and after the 9th day of the study period, no further increase in stool frequency was observed.
Furthermore, as shown in Figure 6, the kombucha group exhibited a mean increase in stool form from baseline, with an increase of þ0.4 points/d and þ1.4 points by the end of the study. In contrast, the control group did not show any significant changes in stool consistency after the 9th day of the study. The differences in stool consistency between the 2 groups were statistically significant at the end of the study (4.4 1.0 compared with 3.4 1.2; P ¼ 0.018). There were no significant changes observed in the results of biochemical blood analysis, blood count, and urine analysis before and after the use of the kombucha drink (Supplemental Table 2).
In the kombucha group, the majority of patients reported good tolerance and found the kombucha drink enriched with
inulin and vitamins to have a pleasant taste. When assessing the palatability of the different flavors using VASs (Table 3), it was observed that by the 14th day of the study, patients rated the taste of the offered drinks similar to the beginning of the study. This indicates that the patients did not become bored with the flavor of the tested drink they had chosen. It is worth noting that the taste score for the mango–passion fruit kombucha drink, as determined by the visual analog scale, was lower compared with the other 2 flavors. However, this decrease in the assessment may be attributed to its association with the occurrence of heartburn in some patients.
Discussion
This pilot study is the first to evaluate the efficacy of an inulinenriched kombucha drink in patients with IBS-C. We showed that a daily serving of the enriched kombucha drink (220 mL) is associated with an increase of stool frequency and an improvement of stool consistency in patients with IBS-C. However, these results need to be validated in a large prospective long-term trial in which patients with IBS-C follow their usual diet, rather than the standardized diet used in our study. The standardized diet in
our study provided all patients with the recommended daily amount of dietary fibers, including inulin for those allocated to the kombucha group. However, in real life, dietary fiber consumption is often much lower. National dietary surveys have shown that intakes of dietary fibers do not meet recommendations, and few countries provide guidance on preferred fiber types to achieve recommended intakes [20]. In Russia, population-based studies have demonstrated that dietary fibers consumption is 30% lower than the recommended 25 g/d [21], and it may be even lower in patients with IBS than in general population.
However, correcting the nutritional patterns associated with IBS-C or any other disease can be challenging because of longestablished food habits and poor long-term compliance with dietary recommendations, especially when it involves the restriction or exclusion of certain foods. To the contrary, regular consumption of specialized/functional food products can contribute to achieving long-term effects with minimal changes to the overall diet structure. However, developing such a product can also be challenging, considering factors such as the type of food product (for example, drink, bakery product, and spread), ease of use, popularity, and the feasibility of modifying the
product's chemical composition. In our study, we chose the drink form for the food product because of its ease of modification and popularity among consumers. There is currently a lack of verified data on the potential long-term health benefits of kombucha itself [22]. However, some findings suggest a potential positive effect of kombucha on various metabolic processes, such as antibacterial and antioxidant effects [23]. This drink holds promise for enriching its composition with water-soluble dietary fibers, such as inulin, which can enhance the interaction of organic acids and other bioactive components of the drink with intestinal receptors. The potential health risks associated with
TABLE 3 Palatability of kombucha drinks with different flavors in patients of the kombucha group (mm VAS)
Flavor Day 5 Day 14 Black currant with juniper 91.0 13.6 94.2 6.5 Strawberry with lime 77.6 27.6 82.7 24.6 Mango with passion fruit 89.5 10.3 87.6 14.1
VAS represented in mm from 0 – “no taste at all” to 100 – “very tasty.” Data are presented as mean SD for normally distributed data. Abbreviation: VAS, visual analog scale.
consuming fermented tea appear to be low and can be mitigated by adhering to proper sanitary practices and manufacturing technology [24]. Inulin was selected for enriching the kombucha-based drink because it has already been widely used for the treatment of constipation and IBS [11–13]. We have previous experience in developing and clinically evaluating inulin-enriched yogurt [25] and dry jelly products [26] enriched with inulin for patients with functional constipation and IBS. However, for the first time, we have developed a kombucha drink enriched with inulin, recognizing the adequate liquid intake is crucial for patients with constipation. Surprisingly, we did not find any studies in patients with IBS utilizing enriched kombucha drinks, although apple juice enriched with inulin was evaluated in patients with constipation [27]. Our decision to create a comprehensive technological process and production cycle of kombucha stemmed from the absence of enriched kombucha drinks in the local market. Furthermore, commercially available products often fail to consistently meet the requirements for permissible ethanol levels, both from batch to batch and even within a single batch, as observed in other countries’ markets [28 30]. This is primarily a result of attempts to economize the fermentation process by reducing its duration, leading to elevated residual ethanol levels in the drink. Furthermore, the high ethanol content can be attributed to improper storage conditions of kombucha within the retail chain. As a solution, we employed our own drink base, which guaranteed all traceability conditions throughout the production, packaging and delivery to patients [19].
The kombucha group showed a significant increase in stool frequency and Bristol stool scale score (BSSS) by day 10 of the intervention, which can be attributed to the effect of inulin, as described in other studies that used inulin supplementation [11 13]. However, the daily dose of inulin in our study was lower than in those previous studies. In the study assessing the efficacy of daily consumption of 300 mL of apple juice enriched with 12 g of highly polymerized inulin in patients with constipation, a significant increase of bowel movements, 1.8 per d, was observed. However, 60% of participants reported occasional abdominal pain during the study [27]. This may be attributed to the high dose of inulin used. In contrast, in our study, we did not observe any differences in abdominal pain, possibly because of the moderate dose of inulin in the kombucha drink.
Although the kombucha drink used in our study underwent pasteurization during the production process [19], rendering it unable to function as a probiotic, we cannot rule out the potential additive positive effects of organic acids and other bioactive components present in the kombucha drink itself. Several experimental studies have demonstrated that acetic, lactic, malic or citric acids can regulate bowel movements through different mechanisms, including the increase of prostaglandin E2 secretion and decreased expression of aquaporin 3 [31,32]. The kombucha drink we utilized in our study contains several organic acids (for example, acetic, malic, citric, lactic, and tartaric) in substantial amounts, which explains the relatively low pH value (3.57) of the drink [19]. When organic acids are ingested with food, they do not reach the colon as they totally absorbed in the small intestine. However, they may stimulate motility and reduce water absorption through mechanisms other than direct changes in pH in the colon lumen. It has been demonstrated that the serum concentration of organic acids in patients with IBS-D is
associated with diarrhea, rather than their content in the feces [33]. Therefore, the organic acids from the kombucha drink may theoretically stimulate intestinal motility and influence constipation in our patients.
By the end of the study, we did not find any differences in other IBS symptoms between the groups, except for the feeling of incomplete bowel emptying, which significantly decreased in the kombucha group. This may be partially explained by the changes in stool consistency observed in this group.
The kombucha-based drink was well tolerated, and we did not observe any changes in urine or blood analyses. The palatability of the drink was evaluated using VAS at the beginning and end of the intervention. Patients rated the taste of kombucha with 2 flavors (black currant with juniper and strawberry with lime) similar at the end of the study compared with the beginning. However, the product with the flavor of mango with passion fruit received lower ratings because of the occurrence of heartburn in a few patients during the intervention period. Interestingly, patients did not experience heartburn when consuming the kombucha drink with the other 2 flavors. There are several possible explanations for this adverse event. First, kombucha is a fermented drink with a pH of 3.57 [19], which can exacerbate heartburn in patients with reflux diseases. However, the medical records of the patients in the kombucha group did not indicate any reflux disease or prescription of proton pump inhibitors. Since the kombucha drinks only differ in flavoring additives, the passion fruit puree included in the composition may be a potential cause of heartburn, as it has been described to have antispasmodic effects by blocking alpha-adrenoreceptors in smooth muscles [34]. We have previously encountered a similar issue with another functional food product that contained menthol as an antispasmodic component, which successfully alleviated intestinal colic and bloating in patients with IBS [35]. However, mint is contraindicated for patients with gastroesophageal reflux disease because of its potential to relax the lower esophageal sphincter. Therefore, it is possible that we observed a similar effect with passion fruit puree in sensitive individuals in this study.
Our study has several limitations, including the short duration of the intervention period (only 10 d) and the relatively small sample size. In addition, the study only included females, so the efficacy of the kombucha-based drink in males with IBS-C needs to be investigated in future trials. The use of a standardized diet during the study allowed us to control for other dietary factors that could influence the outcomes, such as specific foods, additional liquids, or natural laxatives. However, this approach does not provide insight into the efficacy of the kombucha-based drink in real-life scenarios when patients resume their usual diets. Nonetheless, as a pilot study, our findings support the concept that enriching kombucha with inulin is effective for improving constipation in patients with IBS. To obtain more robust and accurate results, larger-scale randomized placebocontrolled trials are needed. The design of these trials needs to be more sophisticated to elucidate the contribution of each component of the enriched kombucha drink to the clinical effects. These trials should include 3 groups of patients with IBS: one group taking enriched kombucha, another group supplemented with the same dose of inulin and vitamins, and a control group receiving nonmodified kombucha. It would also be valuable to assess the blood levels of organic acids to test the
hypothesis regarding their indirect influence on constipation. In addition, extending the intervention period to 3–4 wk under real-life conditions with the usual diet of patients with IBS-C would provide more comprehensive insights.
In conclusion, this pilot study demonstrated that short-term consumption of a pasteurized, fermented, nonalcoholic drink based on kombucha enriched with inulin and vitamins was associated with increased stool frequency, improved BSSS, and a reduction in the sensation of incomplete bowel emptying in females with IBS-C. However, further validation of these findings is warranted through larger scale, randomized, placebocontrolled trials. If such studies can provide substantial evidence, the drink may be recommended for patients with IBS-C.
Author contributions
The authors’ responsibilities were as follows – VAI, VIP: conceptualization; VAI, VIP, AVV, AAK: methodology; VIP: software, validation, and data analysis; VAI, VIP: resources; VIP: writing—original draft; VIP, VAI: writing—review and editing; VAI: supervision, and all authors: read and agreed to the published version of the manuscript.
Funding
The research was funded by the Russian Science Foundation (Project No. 19-76-30014).
Data availability
The data sets used and analyzed for this manuscript can be made available in the future from the corresponding author upon reasonable request.
Conflict of interest
The authors report no conflicts of interest.
Appendix A. Supplementary data
Supplementary data to this article can be found online at https://doi.org/10.1016/j.cdnut.2023.102037.
References
- [1] F. Mearin, B.E. Lacy, L. Chang, W.D. Chey, A.J. Lembo, M. Simren, et al., Bowel disorders, Gastroenterology (2016), https://doi.org/10.1053/ j.gastro.2016.02.031.
- [2] Y.S. Kim, N. Kim, Sex-gender differences in irritable bowel syndrome, J. Neurogastroenterol. Motil. 24 (4) (2018) 544 558, https://doi.org/ 10.5056/jnm18082.
- [3] M.A. Adeyemo, B.M. Spiegel, L. Chang, Meta-analysis: do irritable bowel syndrome symptoms vary between men and women? Aliment. Pharmacol. Ther. 32 (6) (2010) 738 755, https://doi.org/10.1111/ j.1365-2036.2010.04409.x.
- [4] N. Alammar, E. Stein, Irritable bowel syndrome: what treatments really work, Med. Clin. North Am. 103 (1) (2019) 137–152, https://doi.org/ 10.1016/j.mcna.2018.08.006.
- [5] G.J. Holtmann, A.C. Ford, N.J. Talley, Pathophysiology of irritable bowel syndrome, Lancet Gastroenterol. Hepatol. 1 (2) (2016) 133–146, https://doi.org/10.1016/S2468-1253(16)30023-1.
- [6] H.M. Staudacher, K. Whelan, Altered gastrointestinal microbiota in irritable bowel syndrome and its modification by diet: probiotics,
- prebiotics and the low FODMAP diet, Proc. Nutr. Soc. 75 (3) (2016) 306 318, https://doi.org/10.1017/S0029665116000021.
- [7] C. Di Rosa, A. Altomare, V. Terrigno, F. Carbone, J. Tack, M. Cicala, et al., Constipation-predominant irritable bowel syndrome (IBS-C): effects of different nutritional patterns on intestinal dysbiosis and symptoms, Nutrients 15 (7) (2023) 1647, https://doi.org/10.3390/nu15071647.
- [8] T.F. Teferra, Possible actions of inulin as prebiotic polysaccharide: a review, Food Frontiers 2 (4) (2021) 407–416, https://doi.org/10.1002/ fft2.92.
- [9] P. Parhi, K.P. Song, W.S. Choo, Efficacy of inulin supplementation on the growth and survivability of bifidobacterium longum and bifidobacterium breve in model sugar systems, ACS Food Sci. Technol. 2
- [10] D.U. Nagy, K.A. Sandor-Bajusz, B. Body, T. Decsi, J. Van Harsselaar, S. Theis, S. Lohner, Effect of chicory-derived inulin-type fructans on abundance of Bifidobacterium and on bowel function: a systematic review with meta-analyses, Crit. Rev. Food. Sci. Nutr. (2022) 1 18, https://doi.org/10.1080/10408398.2022.2098246.
- [11] L. Collado Yurrita, I. San Mauro Martin, M.J. Ciudad-Cabanas, M.E. Calle-Puron, M. Hernandez Cabria, Effectiveness of inulin intake on indicators of chronic constipation; a meta-analysis of controlled randomized clinical trials, Nutr. Hosp. 30 (2) (2014) 244–252, https:// doi.org/10.3305/nh.2014.30.2.7565.
- [12] A. van der Schoot, C. Drysdale, K. Whelan, E. Dimidi, The effect of fiber supplementationonchronicconstipationinadults:anupdatedsystematic review and meta - analysis of randomized controlled trials, Am. J. Clin. Nutr. 116 (4) (2022) 953–969, https://doi.org/10.1093/ajcn/nqac184.
- [13] O.B. Barboi, I. Ciortescu, I. Chirila, C. Anton, V. Drug, Effect of inulin in the treatment of irritable bowel syndrome with constipation, Exp. Ther. Med. 20 (6) (2020) 185, https://doi.org/10.3892/etm.2020.9315 (Review).
- [14] M. Bellini, S. Tonarelli, F. Barracca, F. Rettura, A. Pancetti, L. Ceccarelli, et al., Chronic constipation: is a nutritional approach reasonable? Nutrients 13 (10) (2021) 3386, https://doi.org/10.3390/nu13103386.
- [15] T. Frieling, J. Heise, B. Krummen, C. Hundorf, S. Kalde, Tolerability of FODMAP reduced diet in irritable bowel syndrome efficacy, adherence, and body weight course, Z. Gastroenterol. 57 (6) (2019) 740–744, https://doi.org/10.1055/a-0859-7531.
- [16] L. Maagaard, D.V. Ankersen, Z. Vegh, J. Burisch, L. Jensen, N. Pedersen, P. Munkholm, Follow-up of patients with functional bowel symptoms treated with a low FODMAP diet, World J. Gastroenterol. 22 (15)
- [17] A. Mullee, D. Romaguera, J. Pearson-Stuttard, V. Viallon, M. Stepien, H. Freisling, et al., Association between soft drink consumption and mortality in 10 European countries, JAMA Intern. Med. 179 (11) (2019) 1479 1490, https://doi.org/10.1001/jamainternmed.2019.2478.
- [18] J. Kim, K. Adhikari, Current trends in kombucha: marketing perspectives and the need for improved sensory research, Beverages 6
- [19] Y. Frolova, V. Vorobyeva, I. Vorobyeva, V. Sarkisyan, A. Malinkin, V. Isakov, A, et al., Development of fermented kombucha tea beverage enriched with inulin and B vitamins, Fermentation 9 (6)
- [20] A.M. Stephen, M.M. Champ, S.J. Cloran, M. Fleith, L. van Lieshout, H. Mejborn, et al., Dietary fibre in Europe: current state of knowledge on definitions, sources, recommendations, intakes and relationships to health, Nutr. Res. Rev. 30 (2) (2017) 149–190, https://doi.org/ 10.1017/S095442241700004X.
- [21] E.A. Pyryeva, A.I. Safronova, [The role of dietary fibers in the nutrition of the population], Vopr. Pitan. 88 (6) (2019) 5 11, https://doi.org/ 10.24411/0042-8833-2019-10059.
- [22] R.M.D. Coelho, A.L. de Almeida, R.Q.G. do Amaral, R.N. da Mota, P.H.M. de Sousa, Kombucha: review, Int. J. Gastronomy Food Sci. 22
- [23] I. Diez-Ozaeta, O.J. Astiazaran, Recent advances in Kombucha tea: microbial consortium, chemical parameters, health implications and biocellulose production, Int. J. Food Microbiol. 377 (2022) 109783, https://doi.org/10.1016/j.ijfoodmicro.2022.109783.
- [24] J.F. de Miranda, L.F. Ruiz, C.B. Silva, T.M. Uekane, K.A. Silva, A.G.M. Gonzalez, et al., Kombucha: a review of substrates, regulations, composition, and biological properties, J. Food Sci. 87 (2) (2022) 503–527, https://doi.org/10.1111/1750-3841.16029.
- [25] V.I. Pilipenko, E.A. Burliaeva, A.K. Shakhovskaia, V.A. Isakov, [Efficacy of using inulin fortified fermented milk products in patients with functional constipation], Vopr. Pitan. 78 (3) (2009) 56 61.
- [26] V.I. Pilipenko, D.A. Teplyuk, A.K. Shakhovskaya, V.A. Isakov, V.M. Vorobyova, I.S. Vorobyova, et al., [Dry jelly concentrate with vitamins and dietary fiber in patients with IBS with constipation: a comparative controlled study], Vopr. Pitan. 84 (6) (2015) 83 91.
- [27] P. Glibowski, M. Skrzypek, M. Cwiklinska, M. Drozd, A. Kowalska, Chemical stability of fructans in apple beverages and their influence on chronic constipation, Food Funct 11 (5) (2020) 3860 3866, https:// doi.org/10.1039/c9fo02596k.
- [28] S.S. Jang, I.L. Mc, M. Chan, P.N. Brown, J. Finley, S.X. Chen, Ethanol concentration of kombucha teas in British Columbia, Canada, J. Food Prot. 84 (11) (2021) 1878–1883, https://doi.org/10.4315/JFP-21-130.
- [29] D. Rossini, C. Bogsan, Is it possible to brew non - alcoholic kombucha? Brazilian scenario after restrictive legislation, Fermentation 9 (9)
- [30] M. Talebi, L.A. Frink, R.A. Patil, D.W. Armstrong, Examination of the varied and changing ethanol content of commercial kombucha products, Food Anal. Methods. 10 (12) (2017) 4062 4067, https:// doi.org/10.1007/s12161-017-0980-5.
- [31] J.R. Na, E. Kim, C.S. Na, S. Kim, Citric acid -enriched extract of ripe Prunus mume (Siebold) Siebold & Zucc. Induces laxative effects by regulating the expression of aquaporin 3 and
- prostaglandin E2 in rats with loperamide - induced constipation, J. Med. Food. 25 (1) (2022) 12 23, https://doi.org/10.1089/ jmf.2021.K.0138.
- [32] L. Wang, S. Cen, G. Wang, Y-k. Lee, J. Zhao, H. Zhang, et al., Acetic acid and butyric acid released in large intestine play different roles in the alleviation of constipation, J. Funct. Foods. 69 (2020) 103953, https:// doi.org/10.1016/j.jff.2020.103953.
- [33] Z. Tian, X. Zhuang, M. Luo, W. Yin, L. Xiong, The propionic acid and butyric acid in serum but not in feces are increased in patients with diarrhea-predominant irritable bowel syndrome, BMC Gastroenterol 20 (1) (2020) 73, https://doi.org/10.1186/s12876-02001212-3.
- [34] S. Patel, T.M. Saleem, V. Ravi, B. Shrestha, N. Verma, K. Gauthaman, Passiflora incarnata Linn: a phytopharmacological review, Int. J. Green Pharm 3 (4) (2009) 277–280, https://doi.org/10.4103/09738258.59731.
- [35] V.I. Pilipenko, D.A. Teplyuk, A.K. Shakhovskaya, V.A. Isakov, V.M. Vorobyova, I.S. Vorobyova, et al., [Using a multicomponent functional food in IBS patients with constipation a comparative controlled study], Vopr. Pitan. 85 (2) (2016) 84 91.
Figures
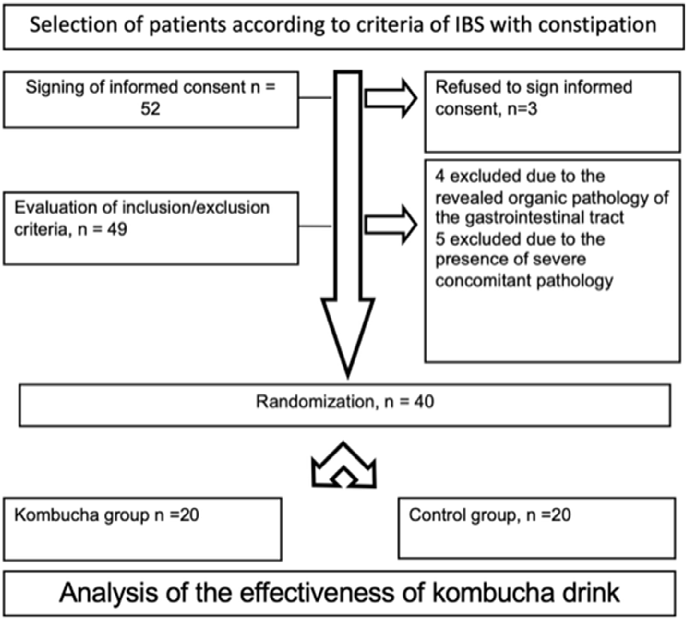
Figure 2
CONSORT flow diagram detailing patient enrollment, randomization, allocation to treatment and control groups, and final analysis in the IBS-C kombucha intervention trial. Dropout rates and reasons for exclusion are documented at each stage.
flowchart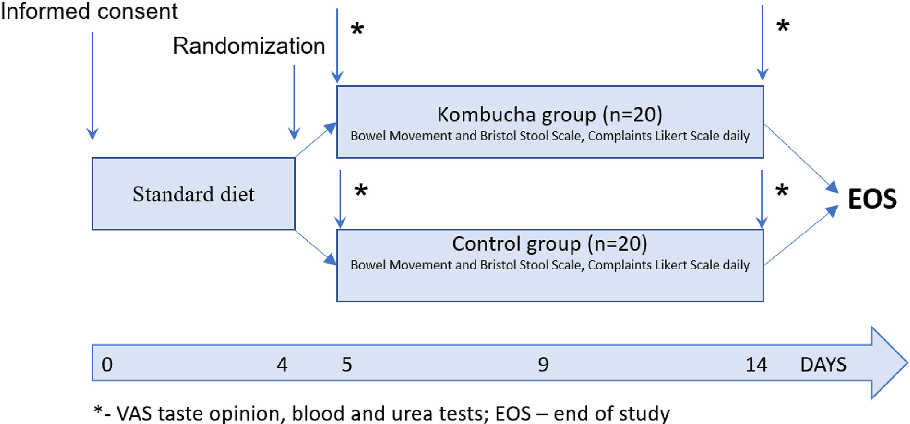
Figure 3
Study design schematic illustrating the intervention protocol, including kombucha drink composition (with inulin and vitamin supplementation), dosing schedule, and assessment timepoints across the trial period.
diagram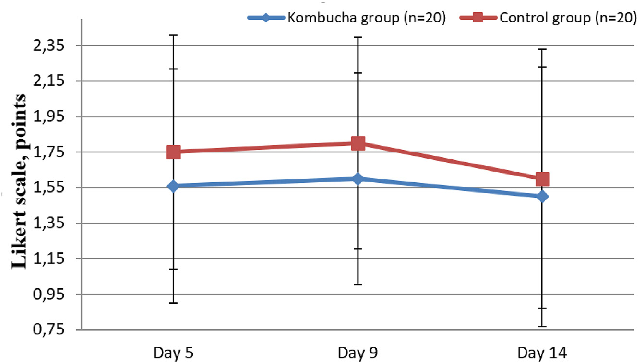
Figure 4
Comparison of bloating severity scores between the kombucha intervention group and control group over the study period. Reductions in bloating severity suggest the enriched kombucha drink may be associated with symptomatic improvement in IBS-C patients.
chart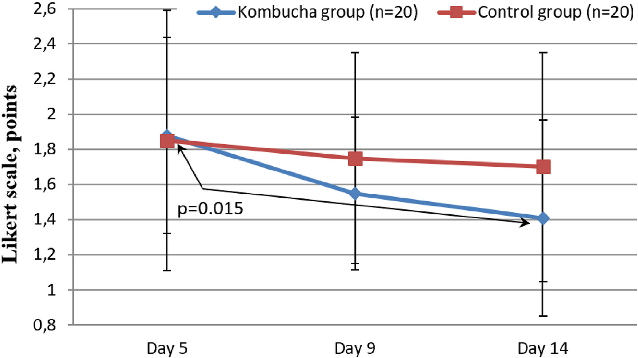
Figure 5
Assessment of the feeling of incomplete bowel emptying in IBS-C patients receiving the kombucha-based drink versus controls. Severity scores at multiple timepoints indicate a trend toward improvement in the intervention group.
chart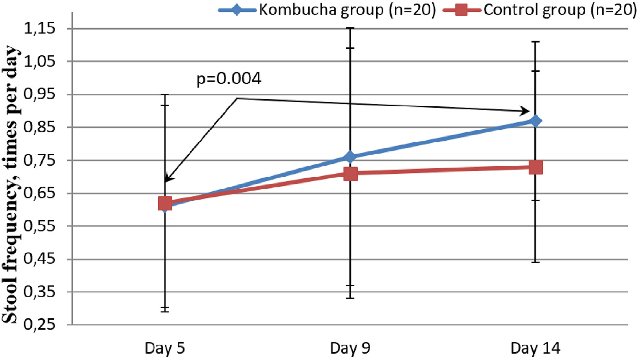
Figure 6
Stool frequency data comparing the kombucha intervention and control groups across the study timeline. Increased bowel movement frequency in the treatment group suggests a potential benefit of the inulin- and vitamin-enriched kombucha formulation.
chart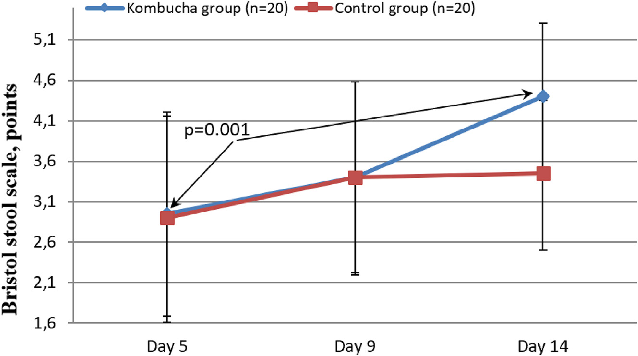
Figure 7
Stool consistency scores evaluated using the Bristol Stool Scale for both study groups. Improvements in stool consistency over the intervention period suggest the kombucha-based drink may help normalize bowel habits in IBS-C patients.
chartUsed In Evidence Reviews
Similar Papers
The American journal of clinical nutrition · 2000
Prebiotics and probiotics: are they functional foods?
Journal of biosciences · 2002
Applications of inulin and oligofructose in health and nutrition.
The American journal of clinical nutrition · 1997
Effects of inulin and lactose on fecal microflora, microbial activity, and bowel habit in elderly constipated persons.
Digestion · 2016
Reduced Abundance of Butyrate-Producing Bacteria Species in the Fecal Microbial Community in Crohn's Disease.
Gut · 2017
Prebiotic inulin-type fructans induce specific changes in the human gut microbiota.
Journal of the Academy of Nutrition and Dietetics · 2017