Colorectal cancer and gut microbiota studies in China.
Study Design
- Tipo de Estudo
- Review
- População
- CRC patients (Chinese studies review)
- Intervenção
- Colorectal cancer and gut microbiota studies in China. None
- Comparador
- None
- Desfecho Primário
- Gut microbiota role in CRC
- Direção do Efeito
- Neutral
- Risco de Viés
- Unclear
Abstract
Colorectal cancer (CRC) is the third most common malignant tumor worldwide. The incidence and mortality rates of CRC have been increasing in China, possibly due to economic development, lifestyle, and dietary changes. Evidence suggests that gut microbiota plays an essential role in the tumorigenesis of CRC. Gut dysbiosis, specific pathogenic microbes, metabolites, virulence factors, and microbial carcinogenic mechanisms contribute to the initiation and progression of CRC. Gut microbiota biomarkers have potential translational applications in CRC screening and early diagnosis. Gut microbiota-related interventions could improve anti-tumor therapy's efficacy and severe intestinal toxic effects. Chinese researchers have made many achievements in the relationship between gut microbiota and CRC, although some challenges remain. This review summarizes the current evidence from China on the role of gut microbiota in CRC, mainly including the gut microbiota characteristics, especially Fusobacterium nucleatum and Parvimonas micra, which have been identified to be enriched in CRC patients; microbial pathogens such as F. nucleatum and enterotoxigenic Bacteroides fragilis, and P. micra, which Chinese scientists have extensively studied; diagnostic biomarkers especially F. nucleatum; therapeutic effects, including microecological agents represented by certain Lactobacillus strains, fecal microbiota transplantation, and traditional Chinese medicines such as Berberine and Curcumin. More efforts should be focused on exploring the underlying mechanisms of microbial pathogenesis of CRC and providing novel gut microbiota-related therapeutic and preventive strategies.
Resumo Rápido
This review summarizes the current evidence from China on the role of gut microbiota in CRC, mainly including the gut microbiota characteristics, especially Fusobacterium nucleatum and Parvimonas micra, which have been identified to be enriched in CRC patients.
Full Text
Colorectal cancer and gut microbiota studies in China
Zikai Wanga,b, Wanyue Dana,c, Nana Zhanga, Jingyuan Fangd, and Yunsheng Yanga,b
aMicrobiota Division, Department of Gastroenterology and Hepatology, The First Medical Center, Chinese PLA General Hospital, Beijing, China; bNational Clinical Research Center for Geriatric Diseases, Chinese PLA General Hospital, Beijing, China; cMedical School, Nankai University, Tianjin, China; dDivision of Gastroenterology and Hepatology, Renji Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai, China
ABSTRACT
Colorectal cancer (CRC) is the third most common malignant tumor worldwide. The incidence and mortality rates of CRC have been increasing in China, possibly due to economic development, lifestyle, and dietary changes. Evidence suggests that gut microbiota plays an essential role in the tumorigenesis of CRC. Gut dysbiosis, specific pathogenic microbes, metabolites, virulence factors, and microbial carcinogenic mechanisms contribute to the initiation and progression of CRC. Gut microbiota biomarkers have potential translational applications in CRC screening and early diagnosis. Gut microbiota-related interventions could improve antitumor therapy’s efficacy and severe intestinal toxic effects. Chinese researchers have made many achievements in the relationship between gut microbiota and CRC, although some challenges remain. This review summarizes the current evidence from China on the role of gut microbiota in CRC, mainly including the gut microbiota characteristics, especially Fusobacterium nucleatum and Parvimonas micra, which have been identified to be enriched in CRC patients; microbial pathogens such as F. nucleatum and enterotoxigenic Bacteroides fragilis, and P. micra, which Chinese scientists have extensively studied; diagnostic biomarkers especially F. nucleatum; therapeutic effects, including microecological agents represented by certain Lactobacillus strains, fecal microbiota transplantation, and traditional Chinese medicines such as Berberine and Curcumin. More efforts should be focused on exploring the underlying mechanisms of microbial pathogenesis of CRC and providing novel gut microbiota-related therapeutic and preventive strategies.
ARTICLE HISTORY
Received 15 December 2022 Revised 28 June 2023 Accepted 10 July 2023
KEYWORDS
Gut microbiota; colorectal cancer; microbial carcinogenesis; microbial biomarkers; anti-tumor therapy; microbiota interventions
Introduction
Colorectal cancer (CRC) threatens the health and causes severe social burdens, accounting for about
- 10% of all new cancer cases.1 Data from the National Cancer Center of China in 2022 showed that CRC ranked fourth in incidence, fifth in mortality among male patients, third in incidence, and fourth in mortality among female patients.2 Europe, Oceania, and northern America have the highest CRC incidence and mortality rate globally. However, recent studies showed that the incidence and mortality of CRC in some regions decreased but increased in China.3 This trend might be influenced by adopting Western dietary and lifestyle patterns and the accompanying alterations in the gut microbiota.4 Improving early diagnosis and
treatment and reducing the disease burden of CRC is a significant public health problem. The gut microbiota plays an essential role in CRC occurrence and progression. This review focally addresses Chinese studies on CRC and gut microbiota to describe the characteristics of the intestinal microbiota associated with CRC, the possible microbial mechanisms, the gut microbiota-related biomarkers for screening, early diagnosis, and risk warnings. It also addresses the role of the intestinal microbiota in chemoradiotherapy and immunotherapy and the application of intestinal microbiota interventions with Chinese characteristics, including microecological agents, fecal microbiota transplantation (FMT), and traditional Chinese medicine (TCM).
CONTACT Yunsheng Yang [email protected] Microbiota Division, Department of Gastroenterology and Hepatology, The First Medical Center, Chinese PLA General Hospital, Beijing, China
© 2023 The Author(s). Published with license by Taylor & Francis Group, LLC. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. The terms on which this article has been published allow the posting of the Accepted Manuscript in a repository by the author(s) or with their consent.
CRC-associated gut microbiota profiles
Intestinal bacterial microbiota and CRC
There are characteristic changes in gut microbiota in various CRC stages, including colorectal adenoma (CRA) and early and advanced CRC.5–8 The CRC cohort-specific noises, like ethnic, geographical, and genetic heterogeneity, might distort the structure of gut microbiota dysbiosis and lead to inconsistent conclusions.5 Searching for a potential core co-set of microorganisms from different cohorts that might be carcinogenic is of great interest to CRC studies.6 Therefore, current studies focused on the gut bacterial microbiota related to CRC across the discovery and validation cohorts based on different ethnic and countries. Unlike CRC patients in Austria, Germany, and France, the gut bacterial composition of CRC patients in China has a unique characteristic with a lower proportion of Firmicutes and a higher proportion of Verrucomicrobia.9 Generally, the characteristics of the intestinal bacterial microbiota of CRC in recent Chinese studies are detailed in
- Table 1. These findings suggest significant differences in the intestinal bacterial microbiota of Chinese CRC patients with respect to different populations,10–14 disease progression15–19 and prognosis.20,21 In the southern Chinese population, the proportion of intestinal Fusobacteria is higher than in Western populations, and CRC in this population may be linked to F. varium and other Fusobacteria species in addition to Fusobacterium nucleatum.22 Several studies from China have integrated the gut metagenomic data of CRC patients among Chinese and other ethnic cohorts and found many bacterial genera, including Fusobacterium, Parvimonas, Peptostreptococcus, Porphyromonas, Gemella, Prevotella, Solobacterium, are associated with CRC. CRCrelated bacterial species include F. nucleatum, Escherichia coli, Bacteroides fragilis, P. micra, P. stomatis, P. ascharolytica, P. somerae, P. intermedia, P. anaerobius, Clostridium symbiosum, S. moorei, and others.5, 23–25 The abundance of F. nucleatum changes in the CRA stage and increases in intramucosal carcinoma and advanced CRC; the relative abundance of Atopobium parvulum and Actinomyces odontolyticus increases significantly multiple CRA and intramucosal cancer
stages.26 The incidence of early-onset CRC has been increasing globally, which could display adverse clinical and histopathological features. The characteristic changes of gut microbiota associated with early-onset CRC are unclear. A few studies on the Chinese population showed that Flavonifractor plautii, Actinomyces, and Schaalia cardiffensis were the critical microbes in earlyonset CRC patients.27,28 Moreover, the diversity of the intestinal bacterial microbiota in left-sided colon cancer is higher than in right-sided colon cancer, and the relative abundance of B. vulgatus and C. perfringens is higher.29
SCFAs
SCFAs, including butyrate, propionate, and acetate, are metabolites generated from the gut microbial fermentation of insoluble dietary fiber and build connections among dietary patterns, gut microbiota, and intestinal function. Many bacteria, such as Clostridium and Bifidobacterium, could transform dietary fiber into SCFAs.45 SCFAs serve as energy substrates of colonic epithelial cells and maintain intestinal homeostasis through several vital biological processes. For example, SCFAs could regulate the metabolism of colonic epithelial cells, enhance gut barrier function, and modulate the immune response of the intestine, and the activation of G protein-coupled receptors and the inhibition of histone deacetylase activity may be the potential mechanisms.46
A high-fiber diet could prevent and reduce the occurrence of CRC, which was associated with the increased abundance of SCFAs-producing bacteria and the raised level of SCFAs in the intestine.46 Moreover, a low-fiber diet results in a lack of butyrate-producing bacteria and a lower level of butyrate in the gut observed in CRA and CRC patients. However, the interaction among SCFAs, the gut microbiota, and CRC is complex. SCFAs could antagonize the proliferation, accelerate the apoptosis of CRC cells, and suppress the inflammation-related CRC carcinogenesis pathways.46 SCFAs reduce the burden of carcinogens such as BAs by activating drug-metabolizing enzymes and inhibiting the degradation of primary BAs to secondary BAs.47 SCFAs also serve as a tumor suppressor to modulate gene expression through epigenetic effects.48 In addition, the dysregulation of SCFAs glucose metabolism could be initiated through the intestinal dysbiosis of CRC, and the interaction between SCFAs transporters and glycolysis might correlate with the initiation and progression of CRC.49
Gut microbiota-derived SCFAs can be potentially applied in CRC prevention and treatment. Supplementation of dietary fiber or postbiotics containing SCFAs might play an essential role in CRC prevention;50 the appropriate formulation and amounts and the efficacy evaluation should be further investigated. Furthermore, several preclinical studies showed that SCFAs-producing bacteria and butyrate could enhance the efficacy of
chemotherapy drugs such as oxaliplatin and irinotecan and improve the response to immunotherapy;51 and then SCFAs could alleviate the adverse effect caused by chemotherapeutic adverse effects such as colitis. Studies based on animal models showed the potential value of intestinal microbiota-derived SCFAs in CRC.52 In-depth investigations are needed before the clinical transformation and application of SCFAs in CRC prevention and treatment.
BAs
Individuals who consume high-fat diets have a higher incidence of CRC. Western diets, including high-fat, red, and processed meat, increase the level of fecal secondary BAs, mostly deoxycholic acid and lithocholic acid. The secondary BAs metabolized by gut microbiota are carcinogenetic factors in CRC development.53 Clostridium and Eubacterium mediate BA-related 7α-dehydroxylation and sulfidation. Elevated levels of secondary BAs exert detrimental tumor-promoting effects via mechanisms such as colonic epithelial barrier function injury, oxidative damage to DNA, inflammation, activation of NF‐κB signaling pathway, and increased cell proliferation.54 Studies also showed that cholecystectomy might be associated with CRC, which may be due to the disruption of BAs secretion and intestinal microbiota imbalance.55 BAs modulate the intestinal microbiota, which regulates the BA pool; the disruption of BAgut microbiota crosstalk contributes to CRC development. However, the synthesis, transport, and metabolism of BAs and the mechanisms of BA-gut microbiota interactions involved in carcinogenesis remain unclear and should be further investigated. Moreover, the modulation of gut microbiota, BAs, and BA-related receptor signaling pathways (such as farnesoid X receptor and G protein-coupled bile acid receptor 1) might be novel therapeutic targets and research frontiers for CRC.56
Hydrogen sulfide (H2S)
H2S is generated from the degradation of foodderived nutrients in the intestine by sulfatereducing bacteria (SRB) such as Desulfovibrio spp. H2S promotes CRC occurrence and development by damaging intestinal epithelial cells, inducing
free radical release, DNA damage, and colonic mucosal inflammation, inhibiting butyrate oxidation, cytochrome oxidase, and DNA methylation57. SRB-related intestinal microbial sulfur metabolism is a potential trigger of CRC. A high-fat and highprotein diet can promote the growth of SRB, metabolizing a large amount of genotoxic H2S related to CRC progression.58 There are elevated intestinal H2S levels in CRC patients, and endogenous and microbial H2S produced by cysteine at CRC sites show an upward trend.59
The microbial pathogenesis of CRC
CRC carcinogenesis involves genetic and environmental factors. Genetic mutations, epigenetic changes, inflammation, immune regulation, and metabolic and hormonal disorders contribute to CRC. The main pathway in colorectal carcinogenesis is the “adenoma-carcinoma sequence,” which describes that most CRC cases are sporadic and progress slowly from normal to dysplastic epithelium to carcinoma throughout years.60 Besides, the gut microbiota is the essential environmental factor contributing to the initiation, progression, metastasis, and CRC outcomes. The intestinal microbiota of CRC patients promotes colorectal dysplasia and tumor formation in a germ-free mouse model, providing evidence for the gut microbiota’s involvement in CRC progression.61 According to available studies, the gut microbiota-related carcinogenic mechanisms of CRC involve an imbalance of intestinal microflora, invasion and colonization of pathogenic microbes, and impaired intestinal barrier function induced by microbial metabolites and virulence factors. The tumor microenvironment is altered by inducing the secretion of proinflammatory cytokines and chronic inflammation surrounding intestinal epithelial cells, activating the Wnt/β-catenin and NF-κB pro-inflammatory signaling pathways and exacerbating intestinal epithelial cell DNA damage, ultimately initiating CRC progression (summarized in Figure 1).
There are two models (“alpha-bug” and “driverpassenger”) of intestinal microbial carcinogenesis related to CRC.62 The alpha-bug model holds Helicobacter pylori in gastric cancer and hepatitis B virus in primary liver cancer stimulates the host to produce inflammatory and immune responses,
- Figure 1. Schematic representation of gut microbiota and their metabolites involved in colorectal carcinogenesis at the cellular and molecular levels. Gut bacteria such as Fusobacterium nucleatum, enterotoxigenic Bacteroides fragilis, Peptostreptococcus anaerobius, pks+ Escherichia coli, and Parvimonas micra, and their virulence factors FadA, B. fragilis toxin, and colibactin contribute to the colorectal cancer (CRC) development by activating different pathways that trigger DNA damage, intestinal inflammation, macrophage polarization, and apoptosis.
proto-oncogene activation, and tumor suppressor gene inhibition.62 Enterotoxigenic B. fragilis (ETBF) -related enterotoxin compromises intestinal epithelial permeability, activation of several tumorinitiating relevant Wnt/β-catenin and STAT3 pathways, and immune responses from persistent Th17 activation, leading to CRC progression.6 The abundance of these so-called promoter bacterial microbes significantly increases in cancer or para-cancerous tissues; however, they appear to decrease during CRC progression. The alpha-bug model does not explain the increased abundance of undifferentiated gut microflora in the early stage of CRC progression. Therefore, a driver-passenger model was proposed to explain the complex changes in the intestinal microbiota associated with CRC.63 For example,
- E. coli and ETBF would be driver bacteria that induce DNA damage in intestinal epithelial cells and trigger inflammation to initiate carcinogenesis. These organisms form a unique tumor microenvironment conducive to increasing opportunistic pathogens called passenger bacteria. These passenger bacteria, such as Streptococcus bovis, S. gallolyticus, Roseburia, and Fusobacterium, might participate in cancer promotion and even competitively inhibit driver bacteria growth. On the other hand, the traditional “adenoma-carcinoma sequence” is the primary pathway for CRC occurrence and development, and the other pathway of colorectal serrated lesions;60 the former involves APC, KRAS, BRAF, TP53, SMAD4, and other gene mutations, while the latter involves CpG island methylation phenotype, MLH1, MGMT, and MSI.64
Research has demonstrated that specific “oncomicrobes” promote CRC initiation and progression, with F. nucleatum, ETBF, pks+ E. coli, and P. micra being extensively studied.6 F. nucleatum activates the TLR4/KEAP1/NRF2 axis and the NFκB signaling pathway, accompanied by inducing M2 macrophage polarization and macrophage infiltration in the tumor microenvironment to promote tumor growth.65 In light of this evidence, a “two-hit” model has been proposed with procarcinogenic features that may initiate CRC development, in which somatic mutations are the first hit and F. nucleatum is the second, exacerbating CRC development after benign cells become cancerous.66 Several Chinese research teams contribute to elucidating the gut microbiota-mediated
pathogenesis of CRC. Fang et al. from Shanghai found that F. nucleatum could activate IncRNA ENO1-IT1 transcription to promote CRC initiation and development and activates the autophagic pathway to promote CRC chemoresistance,67,68 while enterotoxigenic B. fragilis promotes Th17 cell differentiation through downregulation of miR-149-3p. The team proposed for the first time that gut microbiota and host co-metabolism regulate the gut immune microenvironment. The gut microbiota promotes colorectal carcinogenesis by mediating the host urea cycle and disrupting intestinal immune homeostasis.69 Furthermore, Yu et al. from Hong Kong focused on the microbialmediated pathways in CRC. P. micra induces tumors in mice by inducing colorectal cell proliferation and modulating the Th17 immune response,70 while P. anaerobius promotes colorectal tumorigenesis by binding to integrin α2/β1 and activating NF-κB signaling pathway.71
Additionally, many studies focused on the characteristics of the intestinal microbial virulence factors associated with CRC. Gut dysbiosis is carcinogenic through intestinal microbialassociated virulence factors that induce inflammation or immunosuppression. The genetic toxicity of intestinal microbial-associated virulence factors leads to host DNA damage, also involved in CRC initiation and development. The unique FadA adhesin secreted by F. nucleatum binds to E-cadherin (CDH1) and forms a FadA-CDH1Annexin A1-β-catenin complex that activates Wnt/β-catenin signaling to promote initiation and progression of CRC.72,73 F. nucleatum adheres to E-cadherin on the surface of CRC cells and activates the Wnt/β-catenin and NF-κB inflammatory pathways, increasing the proliferation, and invasive activities of CRC cells, promoting metastasis.74 The Fap2 protein of F. nucleatum directly interacts with TIGIT, leading to the bacterium-dependent tumor immune evasion mechanism.75 ETBF, a subtype of B. fragilis, secretes B. fragilis toxin (BFT) to activate the NFκB, STAT3, and Wnt/β-catenin signaling pathways in colonic epithelium cells, triggering inflammation responses and causing excessive cell proliferation; in this way, ETBF promotes carcinogenesis in CRC.76 BFT produces spermidine and H2O2 as byproducts of polyamine catabolism, leading to
apoptosis, inflammation, and DNA damage.77 Colibactin produced by pks+ E. coli strain induces DNA double-strand breaks in host cells through its deoxyribonuclease activity, activating DNA damage signaling cascades and increasing the frequency of gene mutations associated with CRC development.78 Nevertheless, the microbialassociated pathogenesis of CRC and CRA remains to be elucidated. Notably, the research into the pathogenesis of CRC is not limited to several novel pathogenic microbes and their virulence factors to promote CRC initiation and development but continues to advance and deepen.
Gut microbiota-related biomarkers for the screening and early CRC diagnosis
Although the incidence rate of CRC in China is lower than that in Europe and northern America, the number of CRC patients is the largest globally for the large population.3 Most CRC patients are in the middle or late stage of diagnosis and lose the opportunity for surgery, leading to poor outcomes and high mortality rates. The overall burden for CRC diagnosis and treatment remains severe globally. The recent China guideline for the screening and early detection of CRC has recommended that individuals with a high risk of CRC should undergo screening at 40 years of age, and the optimal age for starting CRC screening is 45 years old.79 Colonoscopy is regarded as the gold standard for CRC screening, which could reduce the incidence and mortality of CRC.80 However, as an invasive procedure, colonoscopy is challenging as a large-scale screening method.81 The coverage and participation rate were also lower in China than in America, which limited the effectiveness of nationwide CRC screening.3 In addition, fecal occult blood testing, fecal immunochemical test (FIT), and blood DNA methylation biomarkers are the recommended noninvasive screening methods, which are superior to colonoscopy regarding clinical compliance and cost-effectiveness; nevertheless, they still have limited sensitivity for advanced CRA and CRC.82 Longitudinal studies involving various stages of CRC and cross-sectional studies of different CRC cohorts
suggested that the intestinal microbiota is specific in CRC and its precancerous lesions.5,24,83 This finding provides direct evidence for the potential role of microbial biomarkers in CRC screening and early detection. With the development of multi-omics and bioinformatics artificial intelligence algorithms, innovating noninvasive intestinal microbiota-related biomarkers have become an essential research field in CRC screening and early diagnosis. The intestinal microbiota-related biomarkers for the screening and early diagnosis of CRC in recent Chinese studies are presented in Table 2.
Bacterial biomarkers
Several recent studies have focused on gut microbial-related biomarkers for noninvasive diagnosis of CRC and its precancerous lesions,24,83–85, with significant studies by Chinese scientists. F. nucleatum is the leading candidate bacterial biomarker for early diagnosis, risk, and outcomes prediction.84,85 F. nucleatum abundance in patients with CRC and its precancerous lesions was significantly higher than in the control group, and the level of F. nucleatum was more elevated in cancer and para-cancerous tissues in CRC.86 Changes in the ratio of F. nucleatum to Faecalibacterium prausnitzii and Bifidobacterium in stool samples from CRC patients might identify early CRC.84 A Chinese study found that detecting F. nucleatum DNA in oral saliva was superior to traditional tumor markers such as CEA and CA199 in diagnosing CRC, and F. nucleatum DNA level was related to overall survival and was an independent factor for predicting CRC outcomes.87 Subsequently, quantitative PCR analysis in another Chinese cohort identified F. nucleatum-related butyryl-CoA dehydrogenase and P. micra-related rpoB as discriminators of CRC patients with an area under the ROC curve (AUC) of 0.84; these genes were enriched in patients with early CRC, suggesting that bacteria-related gene markers have the potential for early CRC diagnosis.24 Compared with the culture and identification of specific microbial strains, the quantitative analysis of CRC-specific bacterial genes might improve the sensitivity and specificity of
- Table 2. Gut microbiota-related biomarkers for the screening and early diagnosis of CRC in recent Chinese studies. Authors Cohort Gut microbiota-related biomarkers AUC
Bacterial-related biomarkers Gao et al.23 CRC vs. CRA the combined panel of 12 species (Parvimonas unclassified, Fusobacterium nucleatum, Roseburia intestinalis, Gardnerella
0.994
vaginalis, Peptostreptococcus anaerobius, Peptostreptococcus stomatis, Lactobacillus iners, Gemella morbillorum, Porphyromonas asaccharolytica, Faecalibacterium prausnitzii, Atopobium vaginae, and Parvimonas micra) and three metabolites
Coker et al.18
0.9417 Yang
CRC vs. NC 11 metabolite biomarkers and six bacterial species (F. nucleatum, P. anaerobius, P. micra, Roseburia inulinivorans, Eikenella corrodens, and Xanthomonas perforans)
CRC vs. NC gene 8,122,329 (unknown function from Coprobacillus) 0.930 Chen
et al.20
CRC vs. CRA Eight gut microbiome-associated serum metabolites 0.92
et al.85
Wu et al.24 CRC vs. CRA 24 differential biomarkers (Streptococcus thermophilus TH1435, P. micra, Bacteroides dorei, Clostridium scindens, Erysipelatoclostridium ramosum, Blautia sp., Eubacterium coprostanoligenes group sp., Lachnospira pectinoschiza, Ruminococcaceae UCG-002 sp., Ruminococcus bromii, Porphyromonas sp. HMSC077F02, Porphyromonas sp. 2007b, Eubacterium ruminantium, Tyzzerella 3 sp., Hungatella hathewayi WAL-18680, Blautia faecis, Bacteroides nordii, Lachnospiraceae UCG-010 sp., Eubacterium ventriosum group sp., Streptococcus infantarius, R. intestinalis, Merdibacter massiliensis, Ruminococcus gnavus group sp., Roseburia hominis A2–183) with age and body mass index
0.89
Xie et al.10 CRC vs. NC Combination of Clostridium symbiosum and F. nucleatum abundance with FIT and CEA test 0.876 Hua et al.22 CRC vs. CRA Combination of the top ten species (Butyricimonas synergistica, Agrobacterium larrymoorei, Bacteroides plebeius,
0.8554
Lachnospiraceae bacterium feline oral taxon 001, C. scindens, Prevotella heparinolytica, bacterium LD2013, Streptococcus mutans, L. bacterium 19gly4, and Eubacterium hallii)
Yu et al.12 CRC vs. NC Two gene biomarkers (from F. nucleatum and P. micra) 0.84 Dai et al.5 CRC vs. NC 7 CRC-enriched bacterial biomarkers (B. fragilis, F. nucleatum, P. asaccharolytica, P. micra, Prevotella intermedia, Alistipes
0.80 Liang
finegoldii, and Thermanaerovibrio acidaminovorans)
CRC vs. NC A simple linear combination of four bacteria (F. nucleatum + Clostridium hathewayi + undefined species (labeled as m7)
0.886
et al.86
- Bacteroides clarus)
Fungal-related biomarkers Coker
CRC vs. NC Fourteen fungal biomarkers (Aspergillus flavus, Kwoniella mangrovensis, Pseudogymnoascus sp. VKM F-4518, Debaryomyces fabryi, Aspergillus sydowii, Moniliophthora perniciosa, Kwoniella heavenensis, Aspergillus ochraceoroseus, Talaromyces islandicus, Malassezia globosa, Pseudogymnoascus sp. VKM F-4520, Aspergillus rambelli, Pneumocystis murina, and Nosemia apis)
0.93
et al.36
Gao et al.37 CRC vs. NC Thirteen fungal biomarkers (Phanerochaete chrysosporium, A. flavus, Entomophthora muscae, A. rambelli, fungal sp ARF18, Metschnikowia cubensis, Fusarium pininemorale, Spraguea lophii, Candida versatilis, Lachancea waltii, Taxomyces andreanae, Exophiala mesophila, and Brettanomyces anomalus)
0.757
Viral-related biomarkers Nakatsu
CRC vs. NC Twenty-two viral biomarkers (Orthobunyavirus, Inovirus, Tunalikevirus, L5likevirus, Phikzlikevirus, Betabaculovirus, Sp6likevirus, Sfi21dtunalikevirus, Punalikevirus, Lambdalikevirus, C2likevirus, Mulikevirus, Twortlikevirus, γSphaerolipovirus, Circovirus, Spounalikevirus, Cytomegalovirus, Epsilon15likevirus, N15likevirus, Phikmvlikevirus, Cyprinivirus, and Lymphocryptovirus)
0.802
et al.41
Multi-kingdom biomarkers Lin et al.35 CRC vs. NC Five fungi (Aspergillus kawachii, Rhizophagus clarus, Baudoinia panamericana, A. rambelli, Trichoderma atroviride) and
0.9002
nine bacteria (P. micra, F. nucfeatum, G. morbillorum, Porphyromonas asaccharolytica, Dialister pneumosintes, Anaerostipes hadrus, Romboutsia ilealis, Brachyspira pilosicoli, and Streptococcus safivarius)
Liu et al.9 CRC vs. NC 11 bacterial (F. nucleatum, P. micra, G. morbillorum, Ruminococcus bicirculans, R. intestinalis, Pseudobutyrivibrio xylanivorans, Streptococcus anginosus, and Eubacterium eligens), four fungal (A. rambelli, Sistotremastrum suecicum, T. islandicus, and Aspergillus niger) and one archaeal (Pyrobaculum arsenaticum) biomarkers
0.83
AUC: area under the receiver-operating characteristics curve; CRC: colorectal cancer; CRA: colorectal adenoma; NC: normal controls; rpoB: RNA polymerase subunit β; FIT: fecal immunochemical test; CEA: carcinoembryonic antigen.
CRC screening and early diagnosis, reducing the cost and presenting higher clinical operability. For the bacterial gene marker m3 based on
- F. nucleatum, Lachnochlostridium sp., and C. hathewayi, the sensitivity and specificity for distinguishing CRA were superior to F. nucleatum or the FIT method. The m3 gene combined with F. nucleatum, C. hathewayi, B. clarus, and FIT had a higher diagnostic ability for CRC.88 Furthermore, Fang et al. found that FIT combined with quantitative PCR detection of fecal F. nucleatum DNA improved the sensitivity and specificity in
diagnosing and predicting CRC.89 F. nucleatum IgA and IgG antibody-based assays combined with traditional tumor markers such as CEA and CA-199 are also used for CRC screening.90 Combining gut microbiota-related biomarkers with conventional approaches such as FIT to improve the efficiency of screening and early diagnosis for CRC is essential to the clinical translational application of gut microbiota.88,89
In addition to F. nucleatum, other intestinal bacterial biomarkers are used for screening for CRA and early CRC. Some studies analyzed the
intestinal metagenomic characteristics of CRA, early to advanced CRC at different stages, and revealed characteristic changes of the intestinal microbiota at the precancerous stage of CRC.26 Fang et al. validated a set of gut microbiotabased diagnostic models developed to diagnose laterally spreading tumors, the primary precursor lesions of CRC, with an AUC of 0.92.91 Besides, Yu et al. identified four CRC-enriched bacterial-related genes in Chinese exploratory and Danish validation cohorts and further validated them in French and Australian populations with AUCs of 0.72 and 0.77, respectively.24 A.parvulum and A.odontolyticus were only significantly increased in multiple CRA and intramucosal carcinoma, suggesting that there are specific microbial biomarkers for early screening of CRC precancerous lesions.26 A random forest classifier was constructed with
- 11 bacterial phylotypes to distinguish CRA from the control group. A classifier with 26 bacterial phylotypes was constructed to distinguish CRC from CRA with an AUC of 0.89; this classifier was validated in two independent cohorts with AUCs of 0.78 and 0.84, respectively, and these findings were confirmed in a new cohort using real-time quantitative PCR.83 In addition to screening and early diagnosis of CRC, Wei et al. also validated a set of gut microbiotabased diagnostic models to distinguish the newly developed adenomas from the healthy subjects, which may help prevent cancer recurrence in postoperative patients.92
In recent years, multi-omics research showed the potential of intestinal microbial metabolites in CRC screening and early diagnosis.43,93,94 One study developed an intestinal microbiome-related eight serum metabolites panel to predict CRC and CRA with an AUC of 0.92 in the validation cohort, which was significantly better than tumor markers such as CEA, showing the potential application value of serum metabolites associated with intestinal microbiota in identifying CRC and CRA.93 Through fecal metagenomic and metabolomic analysis of CRA and CRC, at different stages from CRA to CRC, Yu et al. found that norvaline and myristic acid showed an increasing trend, and 20 CRC-enriched metabolites distinguished CRC from CRA and healthy control; further integration of microbial metagenomic data
showed that the ability to distinguish CRC from CRA and healthy control was improved with AUC of 0.94 and 0.92 respectively.44 Moreover, a few studies from China tried to find the gut microbial biomarkers for early-onset CRC.27,28,94 One study showed that multi-omics signatures of early-onset CRC might be associated with enriched F. plauti and increased tryptophan, BAs, and choline metabolism. They constructed a microbiome-derived predictive model based on metagenomic, metabolomic, and KEGG orthology gene markers to detect earlyonset CRC.94 Gut microbial-associated biomarkers have shown significant advantages in the noninvasive diagnosis of CRC, although further validation studies are needed before these biomarkers can be used in clinical practice.
Gut microbiota and anti-tumor therapy in CRC
Intestinal microbiota dysbiosis and specific pathogenic microbes have carcinogenic and pro-tumorigenic
effects. Substantial evidence shows that the gut microbiota is associated with the efficacy or adverse effects of anti-tumor treatments such as chemoradiotherapy and immunotherapy.95 The gut microbiota is a potential biomarker to predict anti-tumor responses and adverse reactions. The gut microbiota regulates the efficacy of anti-tumor therapy and clinical CRC outcomes.
Chemotherapy
The intestinal microbiota influences the efficacy of chemotherapy, drug resistance, and intestinalassociated toxicity. The gut microbiota mediates the anti-tumor effects of chemotherapeutic drugs (e.g., 5-FU, gemcitabine, and platinum) through various mechanisms, including translocation, immunomodulation, metabolism, enzymatic degradation, reduced diversity, and ecological variation.96 The gut microbiota is related to the efficacy of chemotherapy for CRC.97,98 Patients with CRC who respond to chemotherapy have a relatively high abundance of Sutterella and Roseburia; a high abundance of Fusobacterium indicates non-response and poor clinical outcomes.99,100 Moreover, the gut microbiota might be involved in chemotherapy resistance. F. nucleatum is enriched in tumor tissues of recurrent CRC patients after chemotherapy, and the abundance of F. nucleatum negatively correlates with the CRC outcomes. F. nucleatum induces drug resistance to platinum and 5-FU in CRC by affecting tumor cell autophagy.68 A study showed that metronidazole reduced the amount of F. nucleatum and shrank the tumor body, suggesting the application of anti-F. nucleatum before chemotherapy in F. nucleatum-positive CRC patients might enhance chemotherapeutic efficacy.101 F. nucleatum is emerging as a microbial biomarker for predicting chemotherapeutic efficacy, drug resistance, and outcomes and is becoming a therapeutic target for CRC. The composition and function of the gut microbiota are altered by cytotoxic chemotherapeutic agents, further affecting microbial-associated drug metabolism.102 The extent of tumor regression in tumor-bearing mice treated with platinum-based chemotherapy is significantly lower after antibiotic treatment, and germ-free mice do not respond to platinum treatment.103 Platinum induces reactive
oxygen species (ROS) aggregation, the primary anti-tumor mechanism of platinum. However, no apparent ROS aggregation was observed in germfree mice or tumor-bearing mice models treated with antibiotics, suggesting that the intestinal microbiota is involved in platinum-induced DNA damage and tumor cell apoptosis.104 The intestinal microbiota assists platinum in activating tumorrelated inflammatory cells to generate ROS, enhancing the role of platinum in killing tumor cells.103 The influence of intestinal microbial-related metabolites on chemotherapy should not be ignored. For example, butyric acid enhances the antitumor cytotoxic effect of CD8+T cells in vitro and promotes the anti-tumor effect of platinum-based chemotherapeutic drugs.51 Supplementation of probiotics alleviates 5-FU and platinum-related intestinal injuries and adverse reactions.105 Lactobacillus supplementation during chemotherapy in CRC patients treated with 5-FU reduces mortality and improves gastrointestinal symptoms such as diarrhea.106 Furthermore, the gut microbiota modulates irinotecan’s metabolism and adverse effects. Irinotecan is a prodrug of SN-38 used to treat CRC. The incidence of irinotecanrelated grade 3–4 diarrhea is 20%-40%, which affects its anti-tumor efficacy. SN-38 is glucuronidated to SN-38 G by liver enzymes and excreted to the intestine, where intestinal bacterial βglucuronidase hydrolyzes SN-38 G to SN-38, resulting in intestinal mucosal injury and diarrhea.96,107 Probiotic supplementation improves diarrhea and intestinal mucosal damage associated with irinotecan treatment.108 The development of intestinal microbiota biomarkers for predicting the efficacy of CRC chemotherapy and microbial interventions for improving the chemotherapeutic efficacy and adverse reactions need to be further studied.
Radiotherapy
The intestinal microbiota might play a specific role in CRC radiotherapy, influencing radiotherapy’s efficacy and participating in adverse intestinal events such as mucositis and radiation enteritis. Radiotherapy causes significant variation in the structure, diversity, and abundance of the intestinal microbiota, characterized by decreased abundance
of Firmicutes and an increased abundance of Proteus, Ackermann, Fusobacteria, and Bacteroides.102 The abundance of pathogenic microbes in advanced CRC patients after radiotherapy is significantly reduced, while the abundance of beneficial microbes such as Lactobacillus and Streptococcus is increased. The increase of beneficial bacteria may be related to the efficacy of radiotherapy. Bacterial taxa such as Thermi and Sphingomonadaceae identify patients with advanced rectal cancer who have achieved complete pathological response and non-pathological complete response after neoadjuvant chemoradiotherapy.109 Oral microbiota alterations influence the gut bacterial composition within CRC tumors, and oral bacteria such as F. nucleatum migrate to the CRC locus and impair radiotherapy’s therapeutic efficacy and outcomes.110
On the other hand, exposure to high-energy radiation causes intestinal mucosal barrier damage and intestinal crypt cell apoptosis, leading to intestinal dysbiosis and increasing the risk of radiation enteritis.102 After radiotherapy, the high abundance of Clostridia, Rothia, and Koalas might be related to intestinal epithelium inflammatory reactions and barrier dysfunction, which lead to radiation enteritis.111 Regulating intestinal microbiota by supplementing probiotics and FMT might effectively prevent and treat radiation enteritis.112 Bifidobacterium, Acidophilus, Streptococcus, and L. casei alleviate the severity of radiation enteritis.113 The intestinal microbiota is expected to be an interventional target for radiation enteritis.
Immunotherapy
Immunotherapy has been used in hematologic malignancies and immune-sensitive tumors. Immune checkpoint inhibitors (ICIs) have been explored in treating CRC in a subset of CRC patients with MSI-H phenotype.114 For metastatic patients with specific subtypes such as MSI-H or DNA mismatch repair deficiency, immunotherapy can achieve a more sustained therapeutic response,115 and combined use of ICIs prolongs survival in patients with advanced refractory CRC.116 Improving the curative effect and reducing intestinal toxicity is a critical problem in CRC immunotherapy.
Cancer immunotherapy involves the gut microbiota, which plays an essential role in the complex interactions among tumors, the immune system, and ICIs.117 The intestinal microbiota is associated with the efficacy of CRC immunotherapy. ICIs did not inhibit CRC progression in germ-free mice, and the antibiotic treatment weakened the anti-tumor effect of ICIs in mice with normal intestinal microflora.117 The effectiveness of ICIs depends on intestinal microbes such as A. muciniphila, B. fragilis, Bifidobacterium sp., Eubacterium limosum, Faecalibacterium sp., Prevotella sp., and Alistipes shahii. A preclinical study showed that A. muciniphila and Prevotella sp. might play an essential role in maintaining the efficacy of ICIs.117 The abundance and positive detection of the Fusobacterium in non-responders were significantly higher than in responders when combining regofinil with treprizumab to treat refractory and advanced CRC.100 B. fragilis induces dendritic cells to mature and helper T lymphocytes to produce an immune response, then enhance the efficacy of ICIs. Bifidobacterium enhances the killing effect of CD8+T cells on tumors by changing the activity of dendritic cells. The gut microbiota is indispensable for the immune response of immunotherapy, which promotes host immunity, improves the host immune microenvironment, and affects the antigen presentation process, thereby changing the outcome of immunotherapy.118
Intestinal microbiota dysbiosis is involved in ICIs-associated colitis.119 Increases in Bacteroidetes are associated with resistance to ICIs-associated colitis; polyamine transport and vitamin B synthesis pathways are associated with colitis predisposition.120 Intestinal microbiota interventions improve metabolic pathways and immunotherapy’s efficacy.121 A set of 11 commensal bacterial strains enhance the therapeutic efficacy of ICIs in syngeneic tumor models.122 Understanding the mechanisms of the intestinal microbiota in promoting ICIs efficacy or drug resistance, exploring microbiota-related biomarkers, enhancing ICIs efficacy, and treating ICIs-related colitis through microecological interventions are expected to revolutionize tumor immunotherapy.
- Figure 2. Overview of candidates for gut microbiota modulation for the prevention and treatment of colorectal cancer, including diet modulations, microecological agents, fecal microbiota transplantation, antibiotics, and traditional Chinese medicine.
Gut microbiota modulation in the prevention and treatment of CRC
Studies have shown that CRC could be prevented by the intestinal microbiota modulation such as diet interventions, probiotics supplement and antibiotics administration. Moreover, there is mounting evidence that several microecological agents, FMT, and TCM could influence the therapeutic effects and clinical outcomes of CRC by modulating the gut microbiota. Therefore, we discuss the promising gut microbiota modulators that are expected to be applied in the prevention and treatment of CRC (Figure 2).
Diet modulations
Chinese medicine theory holds that “medical and edible food and medicine are from the same root,” and an old Chinese proverb says, “Diseases enter by the mouth.” Diet plays a central role in maintaining intestinal microecological homeostasis, and dietary factors influence CRC. Excessive intake of red meat and processed meat products can increase the risk of CRC, while a high-fiber diet helps prevent CRC.50 A study showed that the abundance of carbohydrate fermentation and butyrate-
producing microorganisms in a native African population was higher; in contrast, more microorganisms related to BAs metabolism were found in African Americans.123 These differences are related to different dietary structures. The intestinal flora structure of African Americans changed significantly after taking the high-fiber, low-fat diet. CRC-related molecular markers were reduced in tissues, suggesting that the high-fiber, low-fat diet inhibits harmful intestinal bacteria, improves the abundance of beneficial bacteria, increases butyrate production and glycolysis capacity, reduces the synthesis of secondary BAs, and reduces the risk of colon epithelial cell carcinogenesis.59 Dietary factors affect CRC occurrence and progression by affecting intestinal microbiota and metabolites. Dietary interventions such as functional food supplements containing probiotics or other ingredients maintain the stability of the intestinal mucus layer and the homeostasis of gut microbiota-host interactions.124
Microecological agents
The role of microecological agents such as probiotics, prebiotics, synbiotics, and even postbiotics in CRC is gradually being recognized. Probiotic
products are subject to significant differences in strains, dosage forms, study populations, evaluation standards, and other factors at home and abroad, and the clinical application of probiotic preparations in China has its unique characteristics. The probiotics approved by the National Health Commission of China for use in humans mainly include Lactobacillus, Bifidobacterium, Enterococcus, Streptococcus, Bacillus, Clostridium, and Yeast at the genus levels.125
Microbiota modulators present a new vision for the prevention and the anti-tumor treatment of CRC. Evidence has suggested that high consumption of yogurt with probiotics moderately reduces the risk of CRA and CRC.126,127 Notably, both L. casei Zhang and L. rhamnosus Probio-M9 probiotic strains from China reduced the development of colon tumors in mice by improving intestinal microbial dysbiosis.128,129 Probiotics inhibit the development of CRC by increasing the abundance of probiotics, inhibiting various pathogenic bacteria, producing SCFAs, down-regulating the expression of pro-inflammatory factors, modulating the immune system, and promoting apoptosis.130 Supplementing probiotics, symbiotics, or yogurt with probiotics for those CRC patients receiving chemoradiotherapy or surgery could lower the complications, such as chemotherapy-related diarrhea/colitis, radiation enteritis, and postoperative adverse events.131,132 Preclinical studies showed that Enterobacteriaceae, Bifidobacterium, and Akkermansia muciniphila could improve the efficacy of CRC immunotherapy.133 Besides, L. rhamnosus ProbioM9 enhances the efficacy and responsiveness of anti-PD-1 immunotherapy, which may be a potential candidate for microecological agents.134 In the future, developing novel microecological agents in adjuvant anti-CRC therapy deserves further anticipation.
FMT
The oldest description of FMT is from Chinese medicine. “Prescription Collection of Fifty-Two Diseases” recorded the use of “golden juice” to treat infectious diseases as early as the Western Zhou Dynasty of China (about the tenth century BC). Dr. Ge Hong, in the Eastern Jin
Dynasty of China (about 1700 years ago), edited the “Prescription Collection of Emergency” and called the FMT preparation “yellow soup,” which was used to treat food poisoning and severe diarrhea.135 FMT is a critical way of modulating the imbalance of gut microbiota by transplanting functional fecal microflora of healthy individuals into the gastrointestinal tract of patients. FMT is primarily used for treating refractory or recurrent C. difficile infections, with a more than 90% cure rate. In addition, there are prospects for therapeutic application in inflammatory bowel disease, functional intestinal disorders, metabolic diseases, and rheumatoid immune diseases.135–137
FMT has become a research hotspot associated with cancer therapy, especially for enhancing the efficacy of ICIs, improving ICIs efficacy, drug resistance, and intestinal toxicity.138,139 Data regarding FMT in CRC are somewhat limited; however, a preclinical study showed that a mixture of 11 commensal bacteria enhanced the activity of ICIs and inhibited tumor growth in a mouse model of CRC.122 A study showed that FMT improved the drug resistance of melanoma patients to ICIs and restored the immunotherapeutic response, possibly related to the activation of T cell activity in tumors.122,138 Currently, many clinical studies are being performed to evaluate FMT for improving the efficacy and treatment sensitivity of ICIs. In addition, FMT modulates the intestinal toxicity of chemoradiotherapy and immunotherapy, including severe chemotherapy-related diarrhea or colitis, radiation enteritis, and ICI-related colitis.112,140 FMT has been used to treat refractory ICIsassociated colitis, and complete remission has been reported after single or multiple FMT.141 Preclinical studies showed that FMT alleviates severe diarrhea and intestinal mucositis associated with 5-FU and platinum in CRC mice.140 FMT improved diarrhea, abdominal pain, hematochezia, and other symptoms associated with radiation enteritis,142 suggesting the value of FMT in reducing radiation-induced toxicity and improving radiotherapy outcomes.112 Nevertheless, in-depth studies are needed before applying FMT to cancer therapy; definitions are needed for indications, donor screening, sample quality control, transplantation timing, and safety of FMT for CRC prevention and treatment.
Antibiotics
Antibiotics have direct bactericidal or bacteriostatic effects on intestinal microflora; however, the relationship between antibacterial drugs and CRC is controversial. A large case-control study showed an association between antimicrobial agents and CRC.143 Theoretically, antibiotics might block its drive effect and inhibit tumor growth for F. nucleatum, E. coli sp., and other CRC-related driver bacteria. Studies found that F. nucleatum in primary lesions and liver metastases of CRC; the number of F. nucleatum in tumors decreased, and tumor growth slowed after treatment with metronidazole, suggesting that antimicrobials may have potential therapeutic value for F. nucleatum infection-related CRC.101 The influence of antibiotics on the gut microbiota and its role in CRC needs to be further studied.
TCM
TCM has a long history of application in preventing and treating CRC as a predominant source of natural medicines and herbal products. In China, TCM has excellent potential to combat colorectal carcinogenesis while reducing the side effects associated with chemotherapy and improving the quality of life of CRC patients. TCM could inhibit CRC development by regulating CRC-related signaling pathways, such as PI3K/Akt, NF-κB, MAPK, and Wnt/β-catenin.144
Accumulating evidence suggests the fundamental role of the gut microbiota in the prevention and treatment of CRC through TCM, with the most frequently studied TCM ingredients being Berberine and Curcumin. A randomized doubleblind controlled trial has demonstrated that Berberine effectively reduces the risk of CRA recurrence, suggesting that it is a promising agent for preventing and treating CRC.145 The specific role of gut microbiota in Berberine’s inhibition of CRC tumorigenesis has been elucidated in a set of studies.146,147 A recent investigation of the fecal microbiota of the CRC mouse model using 16S rRNA profiling identified a significant decrease in microbial richness without loss of diversity and an increase in the relative abundance of beneficial bacteria after Berberine treatment, accompanied
by inhibition of several inflammatory and oncogenic pathways, such as NF-κB pathway.147 Preclinical studies have shown that Berberine inhibits CRC initiation and progression by regulating the intestinal microbiota and modulating the tumor microenvironment.146 Besides, Curcumin is identified as a well-tolerated chemotherapeutic adjuvant to oxaliplatin chemotherapy in patients with colorectal liver metastases. It mediates cell cycle arrest and ameliorates Treg-associated inflammation by regulating gut microbiota to exert anti-tumor effects.148 However, there is a lack of research data on the interactions between TCM and intestinal microbiota in CRC. Future research on the role of TCM in CRC prevention and treatment from the perspective of gut microbiota deserves in-depth study.
Conclusion
In the past decades, the morbidity and mortality of CRC in China have increased, transitioning to developed countries such as Europe and the United States. A large population, unique genetics of multiple ethnic groups, variable environments, lifestyles, and dietary and gut microbiota structures are characteristics of China. Gut microbiota dysbiosis is associated with CRC progression. Some specific microbes contribute to CRC carcinogenesis, including F. nucleatum, pks+ E. coli, ETBF, and P. micra. However, the role of fungi and viruses in CRC needs further investigation. The microbial pathogenesis of CRC involves gut microbiota dysbiosis, invasion and colonization of pathogens, microbial-related metabolites, and virulence, which induce pro-inflammatory signaling pathways and exacerbate intestinal epithelial DNA damage, ultimately initiating CRC progression. However, high-quality in vitro and in vivo validation and in-depth evaluation are needed to clarify the gut microbiota-related mechanisms in the carcinogenesis of CRC. Early diagnosis and prediction by microbial biomarkers are promising research areas with significant clinical translational value. Integrating and optimizing intestinal microbiota-related biomarker panels with traditional clinical methods to improve CRC screening and diagnosis levels is promising and worth digging into. Gut microbiota interventions, including
microecological agents and FMT, hold potential clinical applications to enhance drug efficacy, improve drug resistance, and reduce the severe intestinal toxicity associated with anti-tumor therapy of CRC. Moreover, TCM plays anti-tumor roles in CRC as an adjuvant treatment scheme in China. However, in-depth studies combined with the intestinal microbiota are still needed. Today, international cooperation is essential for searching for gut microbiota-related carcinogenic pathways, biomarkers, and interventional approaches to CRC.
Disclosure statement
No potential conflict of interest was reported by the author(s).
Figures
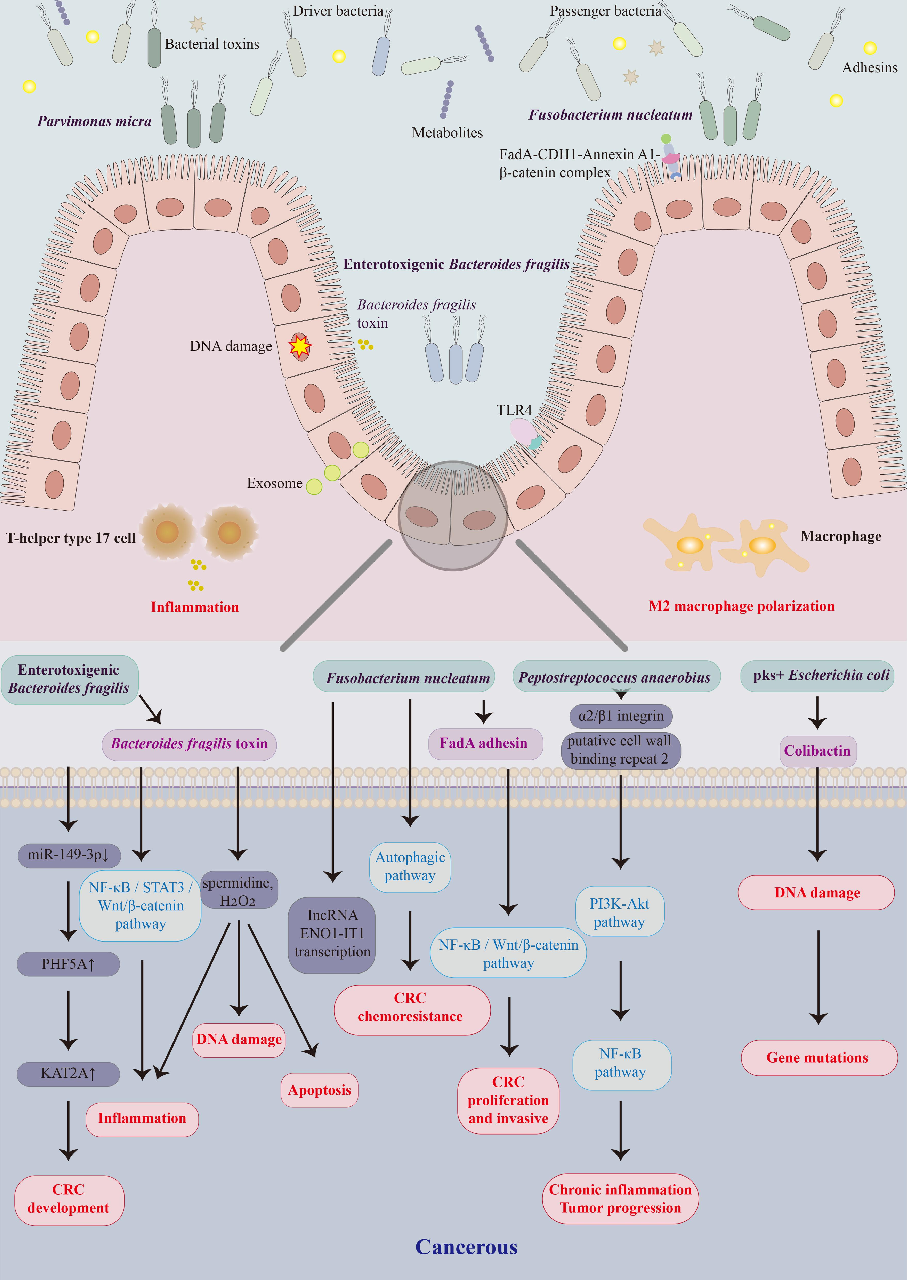
Figure 2
Gut microbiota alterations associated with colorectal cancer in Chinese patient cohorts are characterized, identifying specific bacterial taxa enriched or depleted in tumor-bearing individuals.
chart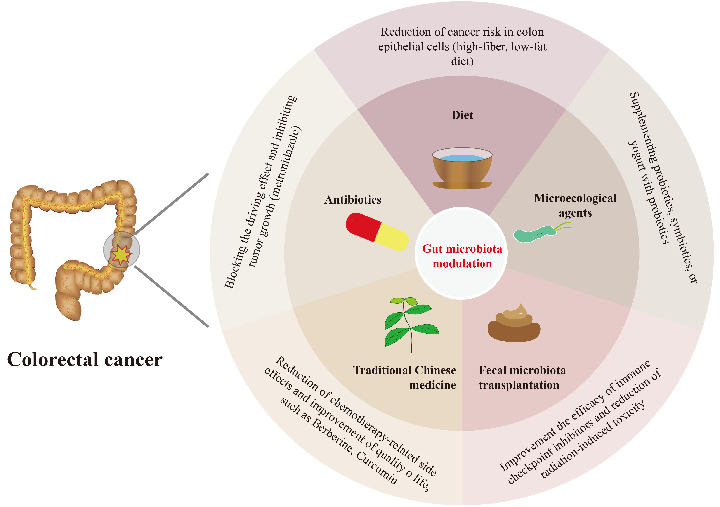
Figure 3
Microbial community composition differences between colorectal cancer patients and healthy controls in Chinese studies are visualized, highlighting potential biomarker species.
chartUsed In Evidence Reviews
Similar Papers
Microorganisms · 2022
Probiotics, Prebiotics, and Phytogenic Substances for Optimizing Gut Health in Poultry.
Pharmacological research · 2021
Main active components of Jiawei Gegen Qinlian decoction protects against ulcerative colitis under different dietary environments in a gut microbiota-dependent manner.
Pharmacological research · 2019
Gut microbiota in phytopharmacology: A comprehensive overview of concepts, reciprocal interactions, biotransformations and mode of actions.
Pharmacological research · 2021
Berberine improves colitis by triggering AhR activation by microbial tryptophan catabolites.
Metabolites · 2023
Phytochemicals and Regulation of NF-kB in Inflammatory Bowel Diseases: An Overview of In Vitro and In Vivo Effects.
American journal of physiology. Endocrinology and metabolism · 2019